Severe endometriosis requires complex surgical and medical treatment to suppress the symptoms that may affect the quality of life of patients with this pathology. We report a case of stage IV endometriosis treated with gonadotropin-releasing hormone (GnRH) agonist after conservative surgery. An 18-year-old nulliparous woman was admitted in our clinic with a history of severe chronic pelvic pain, dysmenorrhea, dyspareunia and dysuria. After a clinical, biological, transvaginal ultrasonography and pelvic CT examination, we diagnosed an rectovaginal endometriosis and bilateral ovarian endometriotic cyst. During laparotomy, a stage IV pelvic endometriosis was found, with bilateral endometrioma of the ovaries, multiple adhesions, deep and superficial lesions of endometriosis. An extensive adhesiolysis, left oophorectomy, right cystectomy and partial omentectomy were performed. For the next 1.5 years, the patient was treated with GnRH for 3 months (goserelin acetate 3.6 mg/month) and then with continuous oral progestin therapy. After 1.5 years, the patient remained asymptomatic, the treatment improving the quality of life. In selected cases, GnRH agonists remains an effective treatment for recurrent symptoms of endometriosis, especially if administered early after surgical therapy.
Agoniştii de Gn-RH în tratamentul endometriozei profunde după chirurgie conservatoare - prezentare de caz
The use of GnRH agonists in deep endometriosis after conservative surgery - case report
First published: 22 mai 2017
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/Gine.16.2.2017.764
Abstract
Rezumat
Endometrioza severă necesită chirurgie complexă şi tratament medical complementar pentru a suprima simptomele care pot afecta calitatea vieţii pacientelor cu această patologie. Prezentăm un caz de endometrioză în stadiul IV tratat cu agonişti de GnRH după tratament chirurgical conservator. Pacienta, în vârstă de 18 ani, nulipară, se internează în serviciul de ginecologie pentru dureri pelviene cronice, dismenoree, dispareunie şi disurie. După bilanţul clinic, biologic, ultrasonografic şi computer-tomografic, s-a stabilit diagnosticul de endometrioză rectovaginală şi endometrioame bilaterale. Intraoperator se constată endometrioză pelviană în stadiul IV, cu endometrioame bilaterale, sindrom aderenţial extensiv pelvian, precum şi leziuni de endometrioză superficială şi profundă. Se practică adezioliză extensivă, ovarectomie stângă, chistectomie dreaptă şi omentectomie parţială. Pacienta a fost supusă unui tratament medical cu goserelin acetat 3,6 mg pe lună şi apoi cu tratament progestativ. După 1,5 ani, pacienta rămâne asimptomatică, cu îmbunătăţirea calităţii vieţii. În cazuri selectate, agoniştii de GnRH reprezintă un tratament eficient pentru prevenirea recurenţelor şi îmbunătăţirea simptomatologiei, în special dacă sunt administraţi ca tratament complementar chirurgiei.
Introduction
Endometriosis is a benign, chronic and estrogen-dependent disease which affects 10% of women during the reproductive period, frequently women between 25 and 35 years old(1,2,3).
Until now, the management of this disorder has remained controversial. The effectiveness of the treatment has been estimated with the evaluation of the pain and infertility. The treatment is intended to eradicate or to limit the extension of the lesions, to improve the symptoms and to delay the relapse. If the medical treatment delays the disease evolution, the surgical treatment tries to eradicate the lesions. The management depends on the severity of the symptoms, the age of the patient and the fertility sparing options(4).
The latest studies have shown that the addition of hormone therapy to surgery increases the period of symptoms improvement and delays the relapse of endometriosis lesions. Also, it has shown a significant improvement of the symptoms after the use of GnRH analogues. These hormones decrease the secretion of FSH and LH, resulting a state of hypogonadotropic-hypogonadism. Reducing the gonadotropic stimulation of the ovaries leads to stagnation of the follicle development and reducing the ovarian steroidogenesis, which decreases the levels of estradiol, the final result being endometrial atrophy and amenorrhea (pseudo-menopausal state)(4).The role of surgery is to diagnose and remove the lesions. The drug treatment promotes the regression/absorption of lesions and limits the extension of the endometriotic implants(4).
Current concepts recommend the treatment with GnRh analogues for 3-6 months after surgery. This management is credited with a good impact on symptoms, particularly improving the pelvic pain syndrome, diminishing the relapse rate and improving the quality of life for patients with endometriosis(5).
Case report
We report the case of an 18-year-old nulliparous woman referred to our hospital with severe chronic pelvic pain, dysmenorrhea, dyspareunia and dysuria. The symptoms started one year ago, and worsened over the last 2 weeks. She had no significant medical or surgical history.
Clinical examination revealed an enlarged abdomen by a tumor (about 15 weeks’ pregnancy), mobile with respiratory movements, painful to palpation and spontaneously, without signs of peritoneal irritation. Clinical examination revealed a normal vulva, vagina and uterine cervix and some blue lesions of the vaginal posterior cul-de-sac, as sign of endometriosis. The uterus was difficult to palpate due to a tumor occupying the lower abdomen.
Ultrasound examination revealed a retroverted uterus of normal size and structure, and three typical images highly suggestive for ovarian endometrioma (right: 7.69/4.65 cm; left: 7.26/4.1 cm, and 7.10/4.48 cm) - Figure 1.
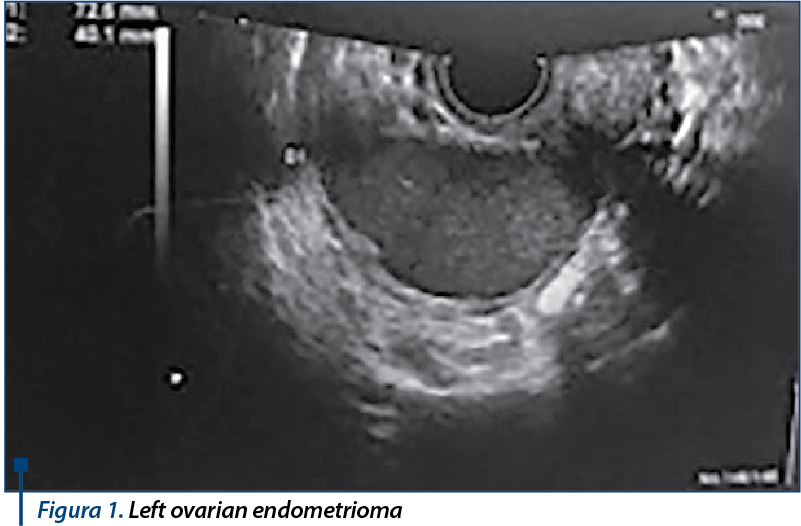
CT scan of lower abdomen and pelvis described a large cystic tumor of 140/74 cm suggestive for endometrioma, belonging to the left ovary and occupying the whole pelvis in close connection with pelvic ureters. Another cystic mass of 84/47 mm, with the same features, was described to the right of middle sagittal plane, in close proximity with the right ureter.
The diagnosis of bilateral endometrioma of the ovaries and rectovaginal endometriosis was established, and laparotomy was decided.
After the opening of the abdomen, we found: a large endometrioma of the left ovary (14/10 cm) with fibrous adhesions to the sigmoid colon and uterus, an endometrioma of the right ovary (6/5 cm), bilateral sactosalpinx, peritoneal endometriosis of the cul-de-sac (powder gun), extensive adhesions in the pelvis and of the omentum to the left ovarian endometrioma.
We performed an extensive adhesiolysis followed by left oophorectomy, cystectomy of the right ovary and partial omentectomy. Multiple peritoneal biopsies were taken. The pathology report confirmed endometriosis in all specimens. The postoperative outcome was uneventful and the patient was discharged in day 4 postoperatively.
The patient received a gonadotropin-releasing hormone for 3 months (goserelin acetate 3.6 mg/month) and then continuous progestin therapies for 14 months. After 18 months from the surgery, the patient remains asymptomatic and the quality of life has improved. The follow-up, at every three months, consisted in clinical examination, vaginal ultrasound and filling a questionnaire (VAS score) in order to assess the presence and severity of pelvic pain.
Discussions and conclusions
Endometriosis is an estrogen-dependent chronic inflammatory disease caused by the growth of functional endometrium tissue outside the uterine cavity. It can be associated with dysmenorrhea, dyspareunia, chronic pelvic pain, and infertility(1).
Endometriosis is the most important cause of chronic pelvic pain, and could highly influence the quality of life in a large number of patients. Traditionally, surgery is considered the gold standard of treatment, but the relapse is frequent. Recurrence rates for endometriomas are reported from 11% to 32% within 1 to 5 years after excision(6). The recurrence rate, even if unpredictable, is higher in patients with advanced stages at surgery and in younger patients. The recurrence can further intensify pain and reduces fertility(6). For this reason, it is very important to prevent recurrences after conservative surgery.
Medical treatment has focused on prevention the cyclic changes of the endometrium by suppressing estrogens and progesterone levels inducing decidualization (progestins), ovarian suppression (GnRH analogues) or chronic anovulation (oral contraceptives). It has been considered that the hormonal treatment promotes the regression/absorption of lesions and limits the extension of the endometriosis implants. Gonadotrophin-releasing hormone analogues, and combined oral contraceptives or progestins are the most frequently used hormonal treatments(4).
The GnRH analogues induce an estrogen-deficient state and suppress endometrial implant growth. GnRH analogues therapy is expensive and is associated with side effects due to the prolonged hypoestrogenic state(4).
GnRh analogues could not be recommended postoperatively in all cases of endometriosis. In some studies, the recurrence of endometriosis disease after surgical treatment occurred later in the group of patients with postoperative administration of GnRH analogues(12). After the administration of GnRH analogues postoperatively, the same studies show an increased asymptomatic period. No effect of this therapy was found regarding the recurrence rate and fertility outcome(13).
In conclusion, the treatment with GnRh analogues 3-6 months after surgery has a positive impact on symptoms, particularly on improving the painful pelvic syndrome and the quality of life for patients with endometriosis.
Bibliografie
2. Gică N, Peltecu G. The effect of surgery on the quality of life in patients with endometriosis. Revista Ginecologia.ro, 2015; 7(Suppl 1):17-9.
3. Plotogea MN, Secureanu FA, Ionescu OM, Ionescu S, Mehedinţu C, Antonovici MR. Episiotomy scar endometriosis. A case report. Revista Ginecologia.ro, 2015; 10 (Suppl 2):45-8.
4. David L Olive, Elizabeth A Pritts. Treatment of endometriosis, N Engl J Med, 2001; 345:266-75.
5. Jee BC, Lee JY, Suh CS, Kim SH, Choi YM, Moon SY. Impact of GnRH agonist treatment on recurrence of ovarian endometriomas after conservative laparaoscopic surgery, Fertil Steril, 2009; 91(1):40-5.
6. Koga K, Osuga Y, Takemura Y, Takamura M, Taketani Y. Recurrence of endometrioma after laparoscopic excision and its prevention by medical management, Front Biosci (Elite Ed) 2013; 1;5:676-83.
7. Granese R, Perino A, Calagna G, Saitta S, de Franciscis P, Colacurci N, Triolo O, Cucinella G. Gonadotrophin-releasing hormone analogue or dienogest plus estradiol valerate to prevent pain recurrence after laparoscopic surgery for endometriosis: a multi-center randomized trial. Acta Obstet Gynecol Scand, 2015; 94:637–45.
8. Descamps P, Andreeva E, Leng J, Salehpour S, Chapron C. The place of gonadotropin-releasing hormone agonists in the management of endometriosis. J Endometr Pelvic Pain Disord 2014; 6:1–11.
9. Batzer FR. GnRH agonist and antagonist: Options for endometriosis pain treatment, J Minim Invasive Gynecol, 2006; 13(6):539-45.
10. Gallagher JS, Feldman HA, Stokes NA, Laufer MR, Hornstein MD, Gordon CM, DiVasta AD. The Effects of GnRHa plus Add-Back Therapy on Quality of Life for Adolescents with Endometriosis: A Randomized Controlled Trial. J Pediatr Adolesc Gynecol, 2017; 30(2):215-22.
11. Lee DY, Park HG, Yoon BK, Choi D. Effects of different add-back regimens on hypoestrogenic problems by postoperative gonadotropin-releasing hormone agonist treatment in endometriosis. Obst Gynecol Sci.. 2016; 9(1):32-8.
12. Dimitrijevic D, Vasiljevic M, Anicic R, Brankovic S, Ristic A, Devic A, Recurrence rate of ovarian endometriosis in patients treated with laparoscopic surgery and postoperative suppressive therapy. Clin Exp Obstet Gynecol. 2015; 42(3):339-43.
13. Daraï E1, Dubernard G, Azoulay C, Barranger E, Antoine JM, Uzan S. Indications of GnRH analogues before and after surgery for endometriosis, Gynecol Obstet Fertil. 2005; 33(12):1014-7.