Medical simulation is widely recognized as a didactic learning tool for students and health care professionals, with the aim to promote and implement measures dedicated to patient’s safety. It is growing rapidly worldwide, becoming part of the curricula in medical schools and medical societies. It represents a useful method of training for rare and complex situations, with catastrophic potential, for which health care professionals have no experience, could not learn it individually and which could overcome them cognitively. Obstetrics is the only specialty in which relevant results on clinical outcome have been demonstrated in the area of great obstetric emergencies. Medical simulation will increase the level of technical competence and communication, will promote an ethical and responsible behavior and a multidisciplinary teamwork. Its end result will be the improvement of patients’ safety.
Rolul simulării medicale în obstetrică
The role of medical simulation in obstetrics
First published: 10 aprilie 2020
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/OBSGIN.68.2.3857
Abstract
Rezumat
Simularea medicală este unanim recunoscută ca o metodă didactică de învăţat pentru studenţi şi profesioniştii din domeniul medical, având scopul de a promova şi implementa măsuri dedicate siguranţei pacientului. Metoda are o dezvoltare rapidă în întreaga lume, devenind parte a curriculumului din universităţi şi societăţi medicale. Simularea medicală reprezintă o metodă utilă pentru situaţii rare şi complexe, uneori cu potenţial catastrofal, pentru care profesioniştii din sănătate nu au experienţă, nu le pot învăţa individual şi care îi pot depăşi cognitiv. Obstetrica este singura specialitate medicală în care s-au obţinut rezultate clinice relevante în domeniul marilor urgenţe obstetricale. Simularea medicală va creşte nivelul competenţei clinice şi al comunicării, va promova un comportament etic şi responsabil şi o activitate de echipă. În final, ea va îmbunătăţi siguranţa pacientei.
Introduction
Medical simulation is widely recognized as a didactic learning tool for students and health care personnel, with the aim to promote and implement measures dedicated to patient’s safety. It is defined, according to the Society for Simulation in Europe (SESAM), as “a technique, not a technology, aimed to change or to augment experiences from the real world, with guided experiences, which evokes or mimic in an interactive way essential aspects of the real world” (David Gaba, 2004).
Medical simulation has been growing rapidly worldwide, the method becoming more and more credible, and spread in the last decades, as centers and university simulation units, hospitals and clinics, both public and private. At the base of this phenomenon, there were numerous studies(1-5) showing that medical simulation could be a valid and useful method for teaching students, nurses, midwives and doctors of different specialties, if some specific conditions are met(6). Medical simulation appeared as an answer to the specific request of modern medicine, which “traditional” teaching methods could not provide as a whole: necessity of standardized methods for training and evaluation of students in the clinical setting, necessity to exercise maneuvers in a safe and controlled environment, necessity to learn and work as a team, necessity to understand and study human factors in medicine(7).
Short history
The beginning of medical simulation is difficult to establish; there are some instruments to exercise clinical maneuvers since antiquity(8). Modern medical simulation started in 1960 in anaesthesia. The first complex simulator, looking like a patient, named SimONE, was built at the University of Southern California. It was destined to teach intubation and was reacting to some drugs, so the students could understand the consequences of pharmacologic treatment and their maneuvers without prejudicing a real patient(9).
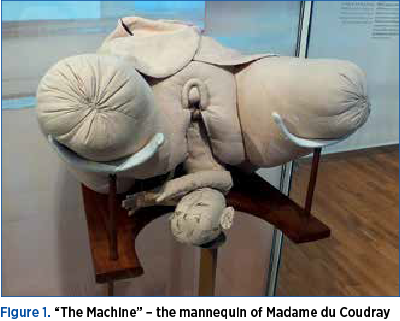
Simulation in obstetrics is documented from the ancient times (Paleolithic), while simulation in gynecology started in the 90s, when the first simulator for laparoscopy – known as “box trainer” – was produced. In the history of medical simulation, a remarkable contribution was made by the midwife Angelique Marguerite du Coudray (1712-1769), who, at the order of kings Louis the XVth and Louis the XVIth, trained 10,000 midwives in 70 cities of France. The simulator model she invented – the first of its kind – was named “The Machine”, and was constructed out of fabric, leather and stuffing, including human bones to form the torso. The female pelvis (birth canal and perineum) and the head of the infant mannequin (shaped nose, stitched ears) were very detailed and accurate (Figure 1). They were very useful to demonstrate the process of childbirth for both cephalic and breech presentation. Madame du Coudray curricula worked hard her students and taught them just the basics. Classes took place six full days a week and lasted around two months, students having plenty of time to listen to lectures and practice each maneuver several times on The Machine. The aim of her training was to reduce the rate of maternal-fetal mortality, which was high both in cities and rural areas(11,12).
Technique and out of fabric for mannequins were considerably diversified in the 20th century. Modern mannequins have the shape and the size of a real woman body, combining functions of intensive care (circulation, respiration etc.) and obstetrics (normal and complicated delivery). A real revolution in the field was represented by Noelle simulator (Gaumard Scientific), capable to virtually reproduce different scenarios of obstetric emergencies destined to train multidisciplinary teams. Today there are many simulators, more advanced technologically, with a higher degree of realism (amniotic fluid, blood loss, mobile joints, monitoring with real equipment, epidural block, wireless order of vital functions and delivery).
Principles and methods used in simulation
At the base of medical simulation are the principles of adult education and numerous teaching theories, one of the most used being the Kolb’s one, referring to the experiential learning. Related to simulation, this theory suggests that an efficient learning takes place when a student experiences a specific situation (i.e., simulation of a postpartum hemorrhage), reflects on his/her actions (mental review of the steps taken), builds alternative concepts (the student draws conclusions about his/her performance and decides what to change in his/her behavior), afterward testing his/her hypothesis (he attends another scenario to improve his/her performance)(13).
Simulation in obstetrics covers three major areas: skills acquisition, periodic training (to review protocols and maneuvers recommended by guidelines of good clinical practice) and exercises performed in situ, meaning the workplace of the beneficiary(14). The methods and equipment used in obstetrics are different, depending on the educational aim and the target group. To fulfill a training of quality it is recommended that the team of instructors and the course director make an analysis of the educational needs of the target group before the course(7).
Another important element is the choice of the simulation equipment, appropriate for different educational objectives. For instance, medical students from the 3rd and the 4th year will use simple simulators, known as anatomical and mechanical models (bladder catheterization, breast palpation), while those in the last year will use simulators of medium fidelity (resuscitation) and actors, known as “standardized patients”. The term “fidelity”, frequently used in simulation, refers to two major aspects: physical and environmental fidelity, which reflects the similarity with the external shape, sensation and functions of the real system (i.e., anatomy of the pelvic canal and the capacity to monitor the patient), and the psychological fidelity that reflects the degree to which the participant perceives the simulation as genuine surrogate for replicated situations (communication to patient and case follow-up)(15).
Usually, high-fidelity simulation with complex and interactive mannequins, performed in environments replicating faithfully a delivery room or an operating theatre, is reserved to medical personnel with good clinical experience and skills. Residents, nurses and midwives could use medical simulation to complete their clinical training for obstetric emergencies and to understand and memorize protocols. Specialists in obstetrics and gynecology use currently medical simulation to consolidate their training in rare, highly specialized or new maneuvers, as well as to optimize teamwork or strategies to prevent critical situations or complications encountered in clinical practice. Some departments use medical simulation to evaluate the performance of their employees in the continuous effort to increase the patient’s safety(16).
A typical day of training with simulation of high fidelity has as first stage of information for all participants the psychological safety, as well as the “rules of the game” in simulation, the presentation of first data about the case selected and distribution of the roles, the development of the actual scenario and, finally, case debriefing. During the development of scenarios, the participants are encouraged to talk to the patient as she would be a real one, and the expected actions are recognizing emergency, asking for help, evaluation of symptoms and signs, initiation of treatment, communication with colleagues and the patient, the stabilization of patient and eventually finding the etiology. During the scenario, vital signs are displayed on the monitor on real time. These could progressively deteriorate or improve, depending on the action of participants. During the scenario there could be added other stress factors, such as fetal distress seen on the CTG. Simulations could be digitally registered and at least one instructor must be present to evaluate objectively (with or without a checklist) the performance of medical teams.
A successful training is the one that favors as much as possible the transfer of knowledge learned in clinical context. A review of the literature showed that this efficiency is depending not only on the performance of simulation equipment, but on multiple factors: clear objectives, realistic and adequate, professional feedback, sustained training (“deliberate practice”), “controlled” learning environment(7).
GEST-URGENT project (POCU/91/4/8/109864), implemented in the Filantropia Cinical Hospital of Obstetrics and Gynecology, Bucharest, Romania, with EU funds, is based on respecting the current recommendations of all societies and foundations in the field (SESAM, Society of Simulation in Healthcare [SSH], PROMPT Maternity Foundation, Scuola Europea di Anestesia Ostetrica [EESOA]), referring to the conduct of a training program on medical simulation in great obstetric emergencies(17-19). The target group was represented by a multidisciplinary team of professionals working in public hospitals in Romania. The type of simulation was a high fidelity one, using the Noelle mannequin (Gaumard Scientific) and different procedural simulators to exercise rare maneuvers (shoulder dystocia, breech lie, neonatal resuscitation, forceps delivery). The goal of scenarios was to increase the confidence of each member of the team, to recognize emergency and its management, learning the clinical algorithm of the given situation, and team communication, following the motto: “Train as a team those you want to work as a team”(20).
Benefits
Obstetrics has the advantage to be the first specialty showing positive and significant clinical results after training on simulation the medical personnel. Remarkable in this respect is a research conducted by Draycott et al. and published in 2005, that studied the incidence of Apgar score ≤6 and perinatal hypoxic ischemic encephalopathy (PIHE) in 19,460 newborns from the Southmead Hospital in Bristol, during a six-year period (1998-2003). The introduction of the training by medical simulation was associated with a significant decrease of incidence of both factors: Apgar score from 86.6 to 44.6 in 10,000 deliveries (p<0.001), and PIHE from 27.3 to 13.6 at 10,000 deliveries (p=0.032). There was a continuous improvement of these factors while the educational intervention continued(21).
Shoulder dystocia
The management of shoulder dystocia showed the most relevant results after the use of medical simulation. Another Draycott’s study(22) revealed an increased frequency of the use of McRoberts’ maneuver from 29.3% to 87.4%, and a decrease of the time of expulsion of the neonate (“head to body delivery time”) from 3 minutes to 2 minutes for cases of dystocia assisted by previously trained teams with a simple simulator device. After training, the risk of neonatal lesions related to shoulder dystocia decreased from 9.3% to 2.3% and that of brachial plexus lesions decreased from 7.4% to 2.3%. The follow-up study at 12 years showed maintenance of positive results, with a special remark that in the last year of study the hospital reported no lesion of brachial plexus on 560 deliveries complicated by shoulder dystocia(23). Similar results were recorded in the USA in 2011, when Grobman et al. implemented a program of management of shoulder dystocia through medical simulation, reporting a decrease in the incidence of the lesions of brachial plexus from 10.1% to 4% (p<0.001)(24).
Postpartum hemorrhage
In Norway (2009-2011), beneficial results were reported related to the implementation of a multidisciplinary simulation program, dedicated to the management of postpartum hemorrhage (>500 ml blood loss when transfusion was recommended), reflected in a significant decrease of the rate of blood transfusion (from 21% in 2009 to 12% in 2011; p<0.01) and of uterine curettage (from 11% in 2009 to 6% in 2011; p<0.01)(25). Significant results were published about a program implemented in 99 hospital in California (The California Maternal Quality Care Collaborative) between 2011 and 2016. This program was developed to standardize procedures of recognition, prevention and management of obstetric hemorrhage. The program included theories and scenarios of medical simulation with standardized checklists and debriefing. A decrease of 20.8% of maternal morbidity associated with bleeding, in the hospitals included in the program, was reported, compared to 1.2% in 48 hospitals that were not included (p<0.0001)(26).
Umbilical cord prolapse
Another study performed in UK, in a third-level maternity teaching hospital, followed the effects of multiprofessional simulation training on the management of cord prolapse for a period of 6 years before (1993-1999) and after (2001-2007). It was observed that diagnosis-to-delivery interval significantly diminished from 25 to 14.5 minutes (p<0.001) and medical teams performed more frequently the therapeutic interventions recommended, as a result of the training (82% after training versus 34% before training; p<0.001). During the posttraining interval, medical teams confronted with 28 cases of cord prolapse and no neonate had an Apgar score <7 at 5 minutes(27). A similar study from Denmark showed similar results on diagnosis-to-delivery interval for emergency caesarean sections(28).
Cardiovascular arrest of pregnant women
Prompt initiation of cardiovascular resuscitation maneuvers and their peculiar aspects related to pregnancy are essentials for a good prognosis on maternal and fetal survival. Simulation has proven to be a useful tool to initiate resuscitation until arrival of advanced support teams (reducing time to initiate maneuvers and to decide caesarean section)(29,30).
Forceps delivery
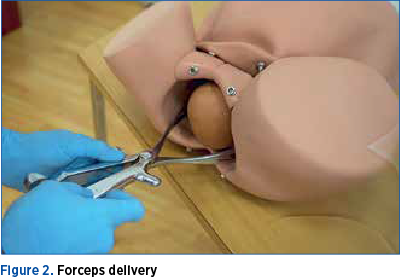
Forceps delivery is an alternative to diminish the rising rates of caesarean sections. Simulation is the best way to train junior doctors. In 2013, Washington University Hospital introduced into the residency program a curriculum of use of forceps based on simulation training, until a level of excellence has been reached (Figure 2). A study period of two and a half years after the training registered a decrease of 26% of the incidence of perineal tears of 3rd and 4th degree associated with the use of forceps (approximately 6000)(31).
Training midwives and students
This showed positive results in recognition and prompt answer to emergencies, neonatal resuscitation, development of professional attitudes based on ethic principles (respect of the autonomy and wish of pregnant woman), cultivate empathy, consolidate self-confidence and relationships with colleagues, and clarify expectations related to professional future(32-37).
Teamwork
The advance in obstetrical simulation is not only technological but conceptual. We are witnessing a change of mentality in the education of health workers: from individual training, based on maneuvers and technical skills, to multidisciplinary teams training through scenarios as realistic as possible and games of roles. This transformation was the result of the request of clinical reality. A report of the 2004 Joint Commission of the United States identified as causes of perinatal deaths and severe disabilities (47) the following: communicating errors (72%), poor competence of staff (47%) and poor training (47%), improper monitoring (40%), lack of resources (30%), lack of supervision (30%), and lack of perinatal information (11%)(38). Simulation is studied as a strategy to improve the efficiency of teamwork, although this aspect is difficult to evaluate. A study performed by Riley et al. compared the results obtained on Weighted Adverse Outcome Score (estimating the total number of adverse events reported to the total number of deliveries) for three hospitals: one hospital receiving only theoretical lectures on team efficiency, one hospital where theory was completed with simulation, and one control hospital, with no didactic intervention. The hospital receiving training simulation had a decrease of perinatal morbidity with 37%(39). At the same time, simulation programs are destined for leadership skill development, compliance, communication, team coordination and processing, and to use information in a team(40).
Limitations
The value of training through medical simulation is recognized by national and international organizations, but its implementation is mainly due to economic aspects and expertise. Training through simulation is different from the mode of education used in universities, based on lectures; it presumes an interactive style, abilities to create scenarios and ensures an optimal climate of learning, group moderator capacities and knowledge about the software of simulation equipment. In order to successfully implement a training with simulation, a support from the management of medical institutions and universities is needed, as well as a clear understanding of the fact that training through simulation aims at educating and improving performance and the results of the team, not at eliminating individual mistakes.
Literature clearly supports that medical simulation is efficient for knowledge acquisition, abilities and attitudes improvement, but at present this shows only moderate effects on clinical results(41). Regarding publications referring to obstetric emergencies, Black and Brocklehurst mention that there are few descriptions of training programs (6 of 44) and even fewer evaluations of them. These authors suggest that researchers’ attention should be paid not so much to answering the question of whether simulation is efficient, but rather to find out how and what make the medical simulation more efficient(42). A meta-analysis of papers on medical simulation highlights that we have to understand how to build more efficient educational programs, how to regulate simulation activity, to standardize curricula and to study the factors influencing the transfer to clinical outcomes(43).
Conclusions
Medical simulation has been used since antiquity and has shown throughout history an added value to education of midwives, doctors and, in the last years, to multidisciplinary teams. It represents a useful training method for rare and complex situations, with catastrophic potential, for which health care professionals have no experience, could not learn it individually, and which could overcome them cognitively. Medical simulation offers a safe and controlled environment, which allows problem-based learning, and competencies are practiced to high standards. The equipment for medical simulation has a wide variety of complexity and is addressed to multiple educational levels, but if you want to get high-quality training for students, a high-quality training of instructors is required. Obstetrics is the only specialty in which relevant effects on clinical outcome have been demonstrated in the area of great obstetric emergencies. Medical simulation will increase the level of technical competence and communication, will promote an ethical and responsible behavior, and a multidisciplinary teamwork. Its end result will be the improvement of patients’ safety.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
1. Khan K, Tolhurst-Cleaver S, White S, Simpson W. Simulation in healthcare education building a simulation programme: A practical guide. AMEE Guide No. 50, 2010.
2. Fernandez R, Vozenilek JA, Hegarty CB, Motola I, Reznek M, Phrampus PE, Kozlowski SWJ. Developing expert medical teams: Toward an evidence-based approach. Acad Emerg Med. 2008; 15: 1025–1036.
3. Gaba DM, Howard SK, Fish KJ, Smith BE, Yasser AS. Simulation-based training in anesthesia crisis resource management (ACRM): A decade of experience. Simul Gaming. 2001; 32: 175–193.
4. Hobgood C, Sherwood G, Frush K, Hollar D, Maynard L, Foster B, Sawning S, Woodyard D, Durham C, Wright M, et al. Teamwork training with nursing and medical students: Does the method matter? Results of an inter-institutional, interdisciplinary collaboration. Qual Saf Health Care. 2010; 19: 1–6.
5. Guise JM, Lowe NK, Deering S, Lewis PO, O’haire C, Irwin LK, Blaser M, Wood LS, Kanki BG. Mobile in situ obstetric emergency simulation and teamwork training to improve maternal-fetal safety in hospitals. Jt Comm J Qual Patient Saf. 2010; 36: 443–453.
6. Issenberg SB, Mcgaghie WC, Petrusa ER, Gordon DJ, Scalese RJ. Features and uses of high-fidelity medical simulations that lead to effective learning: A BEME systematic review. Med Teach. 2005; 27: 10–28.
7. Motola I, Devine LA, Chung HS, Sullivan JE, Issenberg SB. Simulation in healthcare education: A best evidence practical guide. AMEE Guide No. 82. Medical Teacher. 2013; 35:10.
8. Jones F, Passos-Neto CE, Braguiroli OFM. Simulation in Medical Education: Brief history and methodology. PPCR. 2015, Jul-Aug; 1(2):56-63.
9. Improving Education Through: Research, Development, Demonstration, Dissemination, Training, Fiscal Year 1967, Annual Report, Bureau Research. 1968.
10. Nwanodi O. Simulation in General Obstetrics and Gynecology. Journal of Women’s Health, Issues and Care. 2017; 5:6.
11. Carty E. Educating Midwives with the World’s First Simulator: Madame du Coudray’s Eighteenth Century Mannequin. Canadian Journal of Midwifery Research and Practice. 2010; Spring, 9:35-45
12. Rosen KR. The history of medical simulation. J Crit Care. 2008; 23(2):157–66.
13. Kluge A. Experiential Learning Methods, Simulation Complexity and Their Effects on Different Target Groups. Journal of Educational Computing Research. 2007; 36(3), 323–349.
14. Sørensen JL, et al. ‘In situ simulation’ versus ‘off site simulation’ in obstetric emergencies and their effect on knowledge, safety attitudes, team performance, stress, and motivation: study protocol for a randomized controlled trial. Trials. 2013 Jul 17; vol. 14, 220.
15. Sørensen JL. Obstetric simulation: Designing simulation-based medical education and the role of physical fidelity. Interuniversity Center for Educational Research, Maastricht, 2016, p. 15.
16. Daniels K, Lipman S, Harney K, Arafeh J, Druzin M. Use of simulation based team training for obstetric crises in resident education. Simul Healthc. 2008 Fall; 3(3):154-60.
17. Kneebone RL, Nestel D, Vincent C, Darzi A. Complexity, risk and simulation in learning procedural skills. Med Educ. 2007; 41(8):808–14.
18. Dieckmann P, Friis SM, Lippert A, Østergaard D. Goals, Success Factors, and Barriers for Simulation-Based Learning: A Qualitative Interview Study in Health Care. Simulation & Gaming. 2012; 43(5), 627–647.
19. Dieckmann P, Lippert A, Glavin R, Rall M. When things do not go as expected: scenario life savers. Simul Healthc. 2010; 5(4):219–25.
20. Peltecu G, Ban I. Antrenament prin simulare pentru urgenţele obstetricale. Viaţa Medicală. 2014; Available at: https://www.viata-medicala.ro/congrese/antrenament-prin-simulare-pentru-urgentele-obstetricale-9247
21. Draycott T, Sibanda T, et al. Does training in obstetric emergencies improve neonatal outcome? BJOG. 2006 Feb; 113(2):177-82.
22. Draycott TJ, Crofts JF, Ash JP, et al. Improving neonatal outcome through practical shoulder dystocia training. Obstet Gynecol. 2008; 112(1):14–20.
23. Crofts JF, Lenguerrand E, Bentham GL, Tawfik S, Claireaux HA, Odd D, et al. Prevention of brachial plexus injury – 12 years of shoulder dystocia training: an interrupted time-series study. BJOG. 2016; 123:111-118.
24. Grobman WA, Miller D, Burke C, Hornbogen A, Tam K, Costello R. Outcomes associated with introduction of a shoulder dystocia protocol. Am J Obstet Gynecol. 2011; 205(6):513–517.
25. Egenberg S, Øian P, Bru LE, Sautter M, Kristoffersen G, Eggebø TM. Can inter-professional simulation training influence the frequency of blood transfusions after birth? Acta Obstet Gynecol Scand. 2015; 94:316–323.
26. Main EK, Cape V, Abreo A, et al. Reduction of severe maternal morbidity from hemorrhage using a state perinatal quapty collaborative. Am J Obstet Gynecol. 2017; 216:298.e1-11.
27. Siassakos D, Hasafa Z, Sibanda T, Fox R, Donald F, Winter C, Draycott T. Retrospective cohort study of diagnosis-depvery interval with umbipcal cord prolapse: the effect of team training. BJOG. 2009; 116, 1089-1096.
28. Fuhrmann L, Pederson TH, Atke A, Møller AM, Østergaard D. Multidisciplinary team training reduces the decision-to-depvery interval for emergency caesarean section. Acta Anaesthesiol Scand. 2015; 59:1287–1295.
29. Fisher N, Eisen LA, Bayya JV, et al. Improved performance of maternal-fetal medicine staff after maternal cardiac arrest simulation-based training. Am J Obstet Gynecol. 2011; 205:239.
30. Lipman SS, Wong JY, Arafeh J, Cohen SE, Carvalho B. Transport Decreases the Quality of Cardiopulmonary Resuscitation During Simulated Maternal Cardiac Arrest. Anesth Analg. 2013 Jan; 116(1):162-7.
31. Gossett DR, Gilchrist-Scott D, Wayne DB, Gerber SE. Simulation training for forceps-assisted vaginal depvery and rates of maternal perineal trauma. Obstet Gynecol. 2016; 128:429-435.
32. Rakshasbhuvankar AA, Patole S. Benefits of simulation based training for neonatal resuscitation education: A systematic review. Resuscitation. 2014; 85(10), 1320-1323.
33. Kato C, Kataoka Y. Simulation training program for midwives to manage postpartum hemorrhage: A randomized controlled trial. Nurse Educ Today. 2017 Apr; 51:88-95.
34. Buxton M, Phillippi JC, Collins MR. Simulation: a new approach to teaching ethics. J Midwifery Womens Health. 2015 Jan-Feb; 60(1):70-4.
35. Bagnasco A, et al. The role of simulation in developing communication and gestural skills in medicalstudents. BMC Medical Education. 2014; 14:106.
36. Little GN. The Effect of a Simulation Experience on Student Perception of Self Confidence. Nursing Theses and Capstone Projects. 2013; Paper 68.
37. Baptista RC, Paiva LA, Gonçalves RF, Oliveira LM, Pereira MF, Martins JC. Satisfaction and gains perceived by nursing students with medium and high-fidelity simulation: A randomized controlled trial. Nurse Educ Today. 2016 Nov; 46:127-132.
38. The Joint Commission: Sentinel Event Alert: Preventing infant death and injury during depvery. Sentinel Event Alert. 2004; Issue 30, Jul 21.
39. Riley W, Davis S, Miller K, Hansen H, Sainfort F, Sweet R. Didactic and simulation nontechnical skills team training to improve perinatal patient outcomes in a community hospital. Joint Commission J on Quapty and Patient Safety. Aug 2011; 37(8):357-364.
40. Cooper JB, Singer SJ, Hayes J, et al. Design and evaluation of simulation scenarios for a program introducing patient safety, teamwork, safety leadership, and simulation to healthcare leaders and managers. Simulation in Healthcare: journal of the Society for Simulation in Healthcare. 2011; 6:231-8.
41. Zendejas B, Brydges R, Wang AT, Cook DA. Patient Outcomes in Simulation-Based Medical Education: A Systematic Review. J Gen Intern Med. 2013 Aug; 28(8): 1078–1089.
42. Black RS, Brocklehurst P. A systematic review of training in acute obstetric emergencies. BJOG. 2003; 110(9):837–41.
43. McGaghie WC, Issenberg SB, Barsuk JH, Wayne DB. A critical review of simulation-based mastery learning with translational outcomes. Med Educ. 2014 Apr; 48(4):375-85.
Articole din ediţiile anterioare
Stimaţi colegi,
Anul 2023 a început cu activităţi bogate în domeniul obstetricii şi ginecologiei. În luna aprilie, s-a desfăşurat la Bucureşti Primul Congres Naţio...
From safe motherhood to a positive birth experience – times are a-changin’
More then 30 years ago, World Health Organization (WHO) defined “safe motherhood” as a safe, healthy pregnancy and childbirth for all women in the ...
Stimaţi colegi,
Activitatea editorială a Revistei de Obstetrică şi Ginecologie continuă cu subiecte interesante, utile în practica clinică, aflată în continuă evol...
Actualizări privind spectrul de placentă accreta – de la diagnostic la tratament
Spectrul de placentă accreta (PAS), cunoscut şi sub numele de „placenta cu aderenţă morbidă”, reprezintă o entitate patologică ce cuprinde diferit...