Aim. The objective of this study was to evaluate the performance of 3D/4D hysterosalpingo-contrast sonography (HyCoSy) for the assessment of tubal permeability in the infertile patient. Methodology. Tridimensional HyCoSy was performed in a lot of 21 patients diagnosed with primary or secondary infertility, who were referred to our clinic for diagnostic laparoscopy between January and June 2019. Diluted SonoVue® was injected through a 6-8 Fr Foley catheter in the uterine cavity a day before the surgical act. The flow and the spillage of the contrast medium around ovary were recorded using 4D and 3D volumes, and the data were saved for later analysis. The sonographer and the surgical team were blinded regarding patients’ identity and the ultrasound results. The results and the duration of the procedures were noted and compared. Results. Thirty-nine salpinges were evaluated (three previous salpingectomies, two for ectopic pregnancy, one hydrosalpinx), and the overall accordance between 3D/4D HyCoSy and laparoscopic chromopertubation was 84.61%. The sensibility to identify a patent tube was 93.13% and the specificity was 60%. The positive and negative predictive values were 87.1% and 75%, respectively. Conclusions. Hysterosalpingo-contrast sonography using 3/4D acquisition and contrast software is a useful procedure to evaluate tubal patency.
Sensibilitatea şi specificitatea 3D/4D HyCoSy în evaluarea permeabilităţii tubare în context clinic
The sensibility and specificity of 3D/4D HyCoSy to evaluate tubal patency in clinical setting
First published: 16 aprilie 2021
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/ObsGin.69.1.2021.4790
Abstract
Rezumat
Scop. Obiectivul acestui studiu este de a evalua performanţa histerosonosalpingografiei de contrast 3D/4D (HyCoSy) în evaluarea permeabilităţii tubare la pacienta infertilă. Metodologie. La un lot de 21 de paciente diagnosticate cu infertilitate primară sau secundară, internate în clinica noastră pentru laparoscopie diagnostică, în perioada ianuarie-iunie 2019, s-a efectuat histerosonosalpingografie 3D/4D. O soluţie diluată de SonoVue® a fost injectată printr-un cateter Foley 6-8 Fr în cavitatea uterină, cu o zi înainte de actul chirurgical. Fluxul tubar şi revărsarea mediului de contrast în jurul ovarului au fost înregistrate folosind volume 4D şi 3D, iar datele au fost salvate pentru o analiză ulterioară. Rezultatele şi durata procedurilor au fost notate şi comparate. Rezultate. Au fost evaluate 39 de salpinge (trei salpingectomii anterioare, două pentru sarcină ectopică, un hidrosalpinx), iar concordanţa generală între 3D/4D HyCoSy şi cromopertubaţia laparoscopică a fost de 84,61%. Sensibilitatea identificării trompei permeabile a fost de 93,13%, iar specificitatea a fost de 60%. Valorile predictive pozitive şi negative au fost de 87,1%, respectiv 75%. Concluzii. Histerosonosalpingografia de contrast, folosind software de achiziţie şi contrast 3D/4D, este o procedură utilă pentru evaluarea permeabilităţii tubare.
Introduction
Tubal obstruction and pelvic adhesions are common causes of female infertility, accounting for one third of the pathology(1). Repeated pelvic inflammatory disease (PID) is the main cause for the tubal obstruction and the probability to develop infertility is up to 54% after three acute episodes(2). Pelvic inflammatory disease may induce swelling and edema in the fallopian tube, as well as obstruction and enlargement with fluid. It may restrain the normal ovum pick up function of the fimbria of the salpinges, which then leads to fertility issues. Therefore, the evaluation of tubal permeability is mandatory in the diagnosis of female infertility.
In order to evaluate tubal patency, several tests are available, including hysterosalpingography (HSG), laparoscopy with a dye test, selective salpingography and hysterosalpingo-contrast sonography (HyCoSy)(3). HyCoSy is an outpatient ultrasonographic procedure based on the introduction of an ultrasound enhancing positive-contrast fluid into the uterine cavity and the fallopian tubes which can be seen by transvaginal sonography. Despite its benefits, HyCoSy is an operator-dependent process. Precise movements with the probe on transverse plane are essential to identify the passing of liquid through the tube during the injection. The positive-contrast agent highlights the course of the fallopian tubes, producing a hyperechogenic appearance(4). Hysterosalpingography is the conventional modality, for which the diagnostic sensibility and specificity were 65% and 83%, respectively, according to meta-analyses(5). Currently, there are no ultrasonographic dedicated contrast media available for gynecology and recommended by Food and Drug Administration (FDA) and by the European Commission (CE), and the intrauterine and tubal injection is off-label(4,6). Positive second-generation contrast media are considered more stable than saline/air mixture, with better results and the possibility to evaluate the entire tube in the same time using 3D reconstruction(7). These agents provide a substantial harmonic response at low acoustic pressure with better resolution and endure longer than previous contrast agents. The current study was undertaken to compare the concordance of 3D/4D-HyCoSy with the actual gold standard method, diagnostic laparoscopy with metilene dye testing.
Materials and method
The study was approved by the local Ethics Commission for Scientific Study. From January to September 2019, a total of 21 infertile patients scheduled for diagnostic laparoscopy were selected. The inclusion criteria were as follows: proliferative phase of their cycle (days 5-10), no intercourse or use of barrier methods during the cycle, negative vaginal swabs, sterile urine probe, no vaginal bleeding. The exclusion criteria were: acute salpingitis or pelvic inflammatory disease, ultrasound visible tubal pathology (hydrosalpinx), suspected gynecologic tumors, previous extensive gynecologic surgery.
The sonographic exams were performed using the GE Medical Systems, Voluson E8 Expert ultrasound device (equipped with dedicated 4D imaging software program and CCI mode), supplied with a 5-9 MHz transvaginal volume probe. Comprehensive ultrasonic examination was performed in longitudinal and transverse planes and any uterine, fallopian tubes and ovarian abnormalities were observed. A speculum was placed inside the patient’s vagina after betadine disinfection, and a Foley’s catheter (dimension 6-8) was introduced into the uterine cavity with balloon inflated using sterile saline solution (1.5-2 mL) to prevent leakage. The ultrasound probe was reintroduced into the vagina to confirm the position of the balloon after the speculum was taken out. An SF6 microbubble agent (SonoVue®) was used for the preparation of the contrast medium for 4D HyCoSy. Specifically, the content in one SonoVue® vial was suspended with 5 mL of 0.9% normal saline as a first step, which was followed by further dilution of 2.5 mL of the suspension with up to 20 mL of 0.9% normal saline using a 20-mL syringe. The diluted solution of SonoVue® was used in the HyCoSy. Then, using CCI mode, the pelvis imaging became completely anechoic and final 4Dmodality was activated, maintaining the probe fixed in the transverse position. The following criteria need to be followed: 3D box must be placed including the transversal section of uterus and ovaries more than 1 cm for each side (sweep angle maximum 1200); velocity of sweep (medium to maximum quality).
The 4D HyCoSy was started by switching to the scanning mode of 4D contrast-enhanced imaging with the widest region of interest. The contrast medium was injected into the uterine cavity at a stable rate by an assistant. The acquisition of 4D dynamic volume images was triggered immediately at the time of contrast medium visualization in the uterine cavity. The development of contrast in the fallopian tube and overflow from the fallopian fimbria was observed dynamically. The imaging data were saved at 45 seconds by pressing P2 for dynamic storing. The scanning mode was then switched back to 3D contrast enhanced imaging to collect static images, which were saved by pressing P1(8). The multiplanar view of the uterus and tubes, obtained during injection of the contrast medium, was converted automatically, by dedicated software, to the volume image. This resulted in a view of the uterine cavity in coronal section, with both tubes laterally and the contrast medium spilling around the ovaries if both tubes are patent. The dynamic contrast-enhanced volume images were revisited after completion of the contrast-enhanced modes to analyze and observe the contrast flow in the uterine cavity and bilateral fallopian tubes, as well as overflow from the tubal fimbria(8). The patency of the tube was confirmed by the passing of microbubbles (SonoVue® contrast agent) through the tube, the existence of a ring-like spill of free micro bubbles (SonoVue® contrast agent) around the ipsilateral ovary, and the fluid collection in pelvic cavity(9). Circular wrapping (contrast medium encircling more than half of the brim of the ovary) or semicircular wrapping (contrast medium encircling less than half of the brim of the ovary) of the contrast medium could be observed around the ovary (Figure 1).
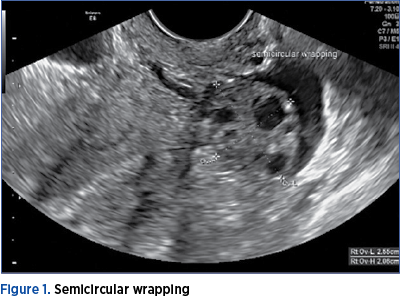
Tubal occlusion at the time of the procedure was positively correlated with the experience of pain and apparent resistance was encountered during injection of the contrast medium. The distal segment of the fallopian tube was in various degrees enlarged and distorted. No overflow of the contrast medium from the ampulo-pavilionar area was noted (Figure 2). In two cases, additional flushing with 10 mL sterile saline was needed to evaluate the flow direction and overflow the liquid from tubal end. After the procedure, all patients received 1 g of single-dose of azithromycin administered orally.
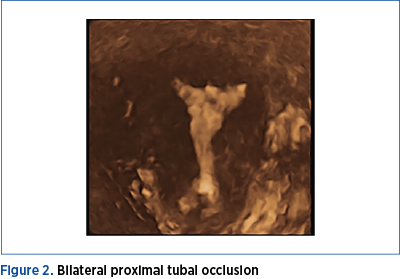
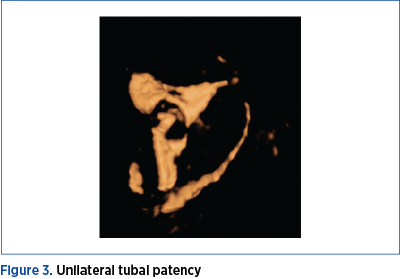
Laparoscopic methylene blue chromopertubation was performed in the next few days, using a larger Foley catheter (12-14 Fr) under general anesthesia and the results were: no resistance during injection, with clear overflow of the solution through tubal fimbria or resistance with obvious reflux and absence of the overflow from the fallopian fimbrial end (Figure 4).
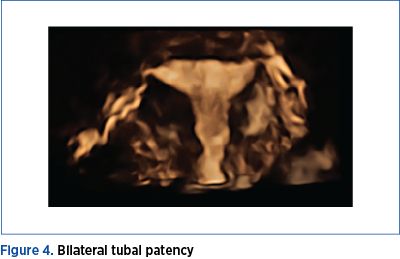

Results
Final tubal permeability status was determined by considering all results, after the completion of the procedure (both 3D and 4D evaluations and all injections), meaning if passage of fluid in the salpinges was observed by either 3D or 4D HyCoSy, we considered the tube patent.
The statistical analysis was conducted to assess whether tubes found to be patent or occluded at 3D/4D contrast imaging HyCoSy had the same status on laparoscopic dye testing. This was done by determining the concordance rate of tubal patency status at the first 4D and at the second 3D volume acquisitions with that at laparoscopic methylene blue dye chromopertubation, by calculating accuracy (percentage concordance). The numeric measurements were summarized as means ± standard deviations (Table 1).
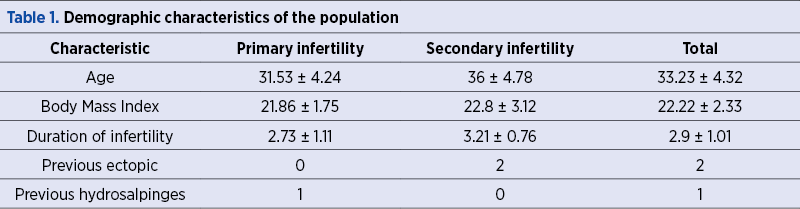
Results of 3D/4D HyCoSy with contrast software for evaluation of tubal patency
There were eight fallopian tubes considered obstructed by 3D/4D HyCoSy, and 31 tubes were patent according to 3D/4D HyCoSy (Table 2). However, we noticed that the contrast medium wrapping around the ovary could be observed during 4D HyCoSy even in obstructed fallopian tubes (two with semicircular wrapping). There were three tubes assessed as patent by 3D/4D HyCoSy that had very little methylene passage according to laparoscopic chromopertubation and were considered patent.

The sensitivity and specificity of 3D/4D HyCoSy with laparoscopic chromopertubation were 93.1% and 60%, respectively. The overall accuracy was 84.61%. The positive and negative predictive values were 87.1% and 75%, respectively (Table 3).

Conclusions
In this study, all 3D/4D HyCoSy were performed in a single center by the same group of physicians, in a similar manner. HyCoSy is an important stage of the assessment of subfertile women, because it can be used to evaluate pelvic pathology, as well as tubal patency. Automated 3D HyCoSy overcame the drawbacks associated with 2D HyCoSy, since is possible to obtain images of the uterus and tubal course that are similar to those obtained by HSG, with the advantage that the image can be moved and rotated in 3D space and also postprocessed in dedicated software. The dynamic character of 4D HyCoSy allows observing the whole process of contrast advancement in real time, but it is a highly operator-dependent technique. The 3D transducer can be moved and rotated at an appropriately slow speed to facilitate the observation of the contrast medium flow in the salpinges, the direction of overflow from the fallopian fimbria, and the process of circular wrapping around the ovary(8). Modern contrast-enhanced ultrasound criteria for the evaluation of tubal patency consider the development of the entire fallopian tube, the overflow of the contrast medium from the tubal end, the circular wrapping of the contrast medium around the ovary, the pelvic spillage, the resistance during injection, and the pain reported by patients comprehensively(8,10,11).
The development of the new contrast medium in conjunction with technical advances of the machine permit better diagnostic results, similar with those of laparoscopic testing, in a cheaper and less invasive approach. In conclusion, 3D/4D HyCoSy is an accurate test for diagnosing tubal patency in women suffering from infertility, whilst overcoming some of the main limitations of other methods(12).
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
- Khalaf Y. ABC of subfertility. Tubal subfertility. BMJ. 2003 Sep 13;327(7415):610-3.
- Muzii L, Sereni MI, Battista C, Zullo MA, Tambone V, Angioli R. Tubo-peritoneal factor of infertility: diagnosis and treatment. Clin Ter. 2010;161(1):77–85.
- Saunders RD, Shwayder JM, Nakajima ST. Current methods of tubal patency assessment. Fert Steril. 2011;95(7):2171-79.
- Exacoustos C, Pizzo A, Lazzeri L, Pietropolli A, Piccione E, Zupi E. Three-dimensional hysterosalpingo-contrast-sonography with gel foam: methodology and feasibility to obtain 3-dimensional volumes of tubal shape. The Journal of Minimally Invasive Gynecology. 2017 Jul-Aug;24(5):827-832.
- Swart P, Mol BW, van der Veen F, van Beurden M, Redekop WK, Bossuyt PM. The accuracy of hysterosalpingography in the diagnosis of tubal pathology: a meta-analysis. Fertil Steril. 1995;64(3):486-91.
- Van Schoubroeck D, Van den Bosch T, Meuleman C, et al. The use of a new gel foam for the evaluation of tubal patency. Gynecol Obstet Invest. 2013;75(3):152–6.
- Doudghene FP, Bazot M, Robert Y, et al. Assessment of Fallopian tube patency by HyCoSy: Comparison of a positive contrast agent with saline solution. Ultrasound in Obstetrics & Gynecology: the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. 2001;18(5):525-30.
- Wang W, Zhou Q, Gong Y, Li Y, Huang Y, Chen Z. Assessment of Fallopian Tube Fimbria Patency With 4-Dimensional Hysterosalpingo-Contrast Sonography in Infertile Women. J Ultrasound Med. 2017 Oct;36(10):2061-2069.
- Li H, Zhang MM, Qiang Y, Ma Y, Mao S, Zhang H. Pain and side effects associated with 4-dimensional hysterosalpingo-contrast sonography for evaluating of the fallopian tubes patency. Computer Assisted Surgery. 2017 Dec;22(sup1):93-99.
- He Y, Geng Q, Liu H, Han X. First experience using 4-dimensional hysterosalpingo-contrast sonography with SonoVue for assessing fallopian tube patency.
- J Ultrasound Med. 2013;32(7):1233–1243.
- Wang SS, Cheng Q, Zhu XS, et al. Value of real time threedimensional hysterosalpingo-contrast-sonography in the assessment of fallopian tube patency. Chin J Ultrason. 2013;22:414–417;
- Wang Y, Qian L. Three- or four-dimensional hysterosalpingo contrast sonography for diagnosing tubal patency in infertile females: A systematic review with meta-analysis. Br J Radiol. 2016;89(1063):20151013.
Articole din ediţiile anterioare
Rolul chirurgiei în cazul pacientelor infertile cu adenomioză
Adenomioza este o maladie benignă ce aparţine unui grup de afecţiuni estrogen-dependente, asociate cu unele consecinţe clinice semnificative: disme...
Tipare de infertilitate. Un studiu de asistenţă medicală primară
Introducere. Infertilitatea reprezintă o problemă medicală şi economică majoră în întreaga lume. Există puţine date referitoare la tiparele cauzelo...
Tratamentul laparoscopic al bolilor pelvine inflamatorii şi implicaţiile infertilităţii
Infecţiile genitale, atât la bărbaţi, cât şi la femei, pot provoca leziuni funcţionale permanente ale aparatului reproductiv, care pot duce la apa...
Managementul histeroscopic al subfertilităţii în cazurile cu suspiciune de polipi endometriali
Polipii endometriali reprezintă o afecţiune ginecologică benignă asociată cu sângerări uterine anormale, infertilitate şi pierderi repetate de sarc...