Introduction. Gynecomastia is the benign development of glandular breast tissue in male patients. Neonatal breast enlargement is a common condition due to postnatal maternal hormones depletion. Firstly, it should be differentiated from mastitis and breast abscess. Recent studies indicate that using progestogen-only contraceptives by breastfeeding women appears to be safe for the breastfed infant. Case report. We report the case of a 2-month-old boy who presented for endocrine evaluation for asymmetric gynecomastia, which had been observed since birth, but left breast enlargement worsened in the last two weeks, overlapping the beginning of mother’s treatment with the contraceptive desogestrel. Hormonal evaluation revealed a slight increase in prolactin values, with normal gonadal, adrenal and thyroid gland hormones. Breast ultrasound showed bilateral glandular breast tissue, without signs of breast abscess. The patient was managed in a multidisciplinary team and had a good clinical evolution, with the resolution of gynecomastia without a particular treatment. Conclusions. We present herein the case of a male infant who was evaluated for bilateral breast enlargement, diagnosed as neonatal gynecomastia, overlapping the mother’s treatment with progestogen-only contraceptive desogestrel, who was followed-up, without a particular treatment, with the resolution of breast enlargement.
Diagnostic challenges in neonatal gynecomastia – case report
Capcane de diagnostic în ginecomastia neonatală – prezentare de caz
First published: 30 iunie 2022
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/Pedi.66.2.2022.6620
Abstract
Rezumat
Introducere. Ginecomastia reprezintă dezvoltarea benignă a ţesutului mamar glandular la pacienţii de sex masculin. Mărirea în perioada neonatală a sânilor este o afecţiune frecventă datorată epuizării hormonilor materni postnatali. În primul rând, trebuie diferenţiată de mastită şi de abcesul mamar. Studii recente indică faptul că utilizarea contraceptivelor numai cu progesteron la femeile care alăptează pare a fi sigură pentru copil. Raportare de caz. Prezentăm cazul unui băieţel în vârstă de 2 luni, care s-a prezentat pentru evaluare endocrinologică pentru ginecomastie asimetrică, observată încă de la naştere, dar mărirea sânului stâng s-a agravat în ultimele două săptămâni, suprapunându-se peste începerea tratamentului mamei cu anticoncepţionalul desogestrel. Evaluarea hormonală a evidenţiat o uşoară creştere a valorilor prolactinei, cu valori normale ale hormonilor gonadali, suprarenali şi tiroidieni. Ecografia mamară a evidenţiat ţesut mamar glandular bilateral, fără semne de abces mamar. Pacientul a fost gestionat în cadrul unei echipe multidisciplinare şi a avut o evoluţie clinică bună, cu rezolvarea ginecomastiei fără un tratament particular. Concluzii. Autorii prezintă cazul unui sugar de sex masculin care a fost evaluat pentru mărirea glandelor mamare bilateral, diagnosticat ca ginecomastie neonatală, suprapusă peste tratamentul mamei cu un contraceptiv conţinând numai progesteron (desogestrel), care a fost monitorizat şi la care nu a fost iniţiat niciun tratament, fiind urmărit, cu rezoluţia măririi sânilor.
Introduction
Gynecomastia is the excessive benign development of breast glandular tissue in male patients. Physiological gynecomastia classically occurs in three age groups: newborns, adolescent boys and older men, involving hormonal changes(1).
Neonatal breast enlargement is a physiological transient response to diminished levels of maternal estrogen at the end of pregnancy, which activates the secretion of prolactin from the newborn’s hypophysis gland(2). However, it is possibly related to placental transformation of androgens to estrogens, which enter the fetal circulation and stimulate glandular breast proliferation(3).
In addition, neonatal breast enlargement is frequent and can be observed in approximately 70-80% of neonates and is independent of the sex of the infant, occurring both in males and females(2).
Breast enlargement usually develops in the first few days of life and resolve spontaneously within weeks to months, without a specific treatment. Furthermore, it is sometimes associated with a milky nipple discharge called “witch’s milk”, maintained and aggravated by squeezing the breast(4).
Continued compression of the breast without parental guidance can result in inflammation, further enlargement, persistence of hypertrophied tissue, and possible infection (mastitis or abscess)(2,5,6).
In addition, overlapping hormonal contraceptive treatment of the breastfeeding mother may play a role in the pathophysiology of breast hypertrophy in the breastfed infant.
Case report
We present the case of a 2-month-old infant referred for endocrine evaluation from the pediatric surgery service for bilateral asymmetric gynecomastia.
He was born at term, at 39 weeks of gestation, by caesarean section, after uncomplicated pregnancy, with a birth weight of 3750 g, and with 9 and 10 Apgar scores at 1 minute and 5 minutes, respectively. He is the second child of the family. He was exclusively breastfed and showed no signs of discomfort or irritability. The parents denied using creams or body oils with xeno- or phytoestrogens.
Bilateral gynecomastia was noticed by the parents since birth, but the breasts continued to grow, with significant enlargement of the left breast, with accentuation in the last two weeks, which coincided with the start of desogestrel progestogen-only pill treatment by the mother, on the recommendation of the gynecologist, after resumption of mothers’ menstruation.
Firstly, on the presentation to the pediatric surgery department, the infant was in good clinical condition, without rash, without signs of staphylococcal skin disease and without fever. The surgeon recommended the application of a local compress with iodine solution to the left breast, until the paraclinical investigations was finished (Figure 1).

Secondly, on the clinical endocrinological exam, the infant had normal anthropometric parameters corresponding to age, with bilateral asymmetrical gynecomastia with prominence of the left breast, corresponding to Tanner stage 2b, with normally colored areolas, with no evidence of tenderness or discharge. In addition, the infant had no particular phenotypic features, with pubertal development corresponding to stage 1 Tanner, with normally conformed penis, without scrotal hyperpigmentation, without pathological pubic hair, and without café-au-lait spots.
The paraclinical examinations showed normal parameters, with normal white blood cells, WBC count = 6400/mm3 (range: 4000-10000/mm3), and normal C-reactive protein (CRP) level (CRP<0.5 mg/dL; normal range <0.5 mg/dL), with no biological inflammatory syndrome.
Hormonal evaluation showed normal gonadotropins, adrenal, testosterone, estradiol and thyroid values, but with slight hyperprolactinemia (prolactin level 20 ng/ml; normal range 4-17 ng/ml).
Ultrasound evaluation of the breasts showed bilateral retroareolar mammary glandular tissue, in the left breast with the size of 2.4/1 cm and 0.5/0.7 cm, respectively, in the right breast, without axillary adenopathy and without any ultrasound sign of mammary abscess (Figure 2).
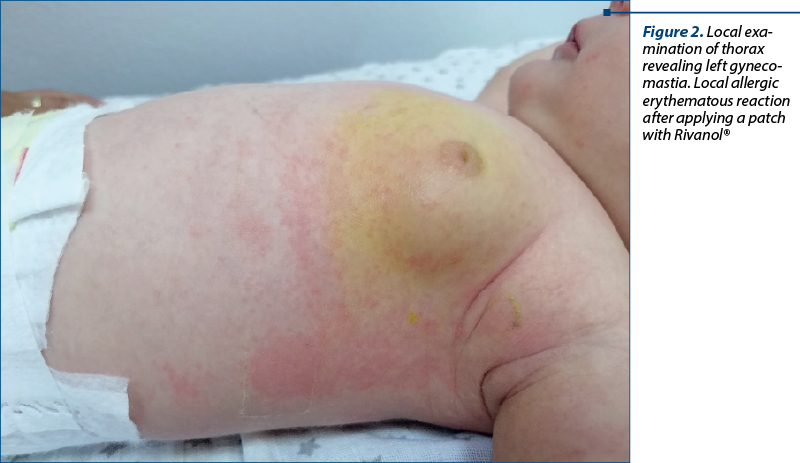
The infant’s case was managed in a multidisciplinary team of pediatrician, surgeon and endocrinologist. Correlating clinical, paraclinical and ultrasound data, we were able to exclude the diagnosis of mastitis or breast abscess and the final diagnosis was neonatal gynecomastia, which overlapped or possibly interfered with the mother’s hormonal contraceptive treatment. Consequently, it was decided to discontinue the mother’s contraceptive medication for a period of time, to continue breastfeeding and monitor the baby without any special treatment. In addition, the parents were informed to avoid squeezing the breast and that a milky discharge might occur. The clinical evolution was favorable, with almost the complete remission of gynecomastia within six months of follow-up.
Discussion
Gynecomastia is a benign growth of male glandular breast tissue and is a common condition in the pediatric population, especially in newborns and young infants(3,7). The most common cause of gynecomastia is an imbalance between androgens and estrogens. One of the incriminated pathophysiological mechanisms is the placental transformation of dehydroepiandrosterone (from fetal and maternal sources) to estrone and estradiol which enter the fetal circulation and stimulate glandular breast enlargement(3). Furthermore, breast tissue hypertrophy is due not only to the effects of pregnancy hormones, but also to the endocrine system activity of the infant, gestational age being one of the factors in determining the normal breast tissue size(8,9). Although the presence of neonatal breast tissue is benign, its persistence and aggravation can be a source of concern(8,10).
In addition to hormonal changes in the mother and newborn, a factor that also influences the appearance and persistence of gynecomastia is the administration of hormonal treatment to the breastfeeding mother. In recent studies and in a systematic review, it has been shown that the administration of progestogen-only methods among postpartum women while breastfeeding is safe for infants, who have normal growth and development in the first years of life(11-13). It is also proven that the use of progesterone preparations does not influence milk production and it was not found any decrease in weight gain of the infant, unlike estrogenic or combined oral contraceptives which are known to decrease the amount of breast milk and produce an unsatisfactory weight gain of the infant(14-16). Even though studies show that the quantity and quality of milk are not modified, two cases of gynecomastia in infants whose mothers received desogestrel-containing progestogen-only pill have been described in literature, but without being able to establish a statistically significant link between the increased breast tissue and the desogestrel pill administration(11,15,17). In addition, the results concluded that neither the treatment with progestogen-only methods had an adverse impact on the health and development of the infants(11,15,17). However, further studies are required to study the exact mechanism by which desogestrel can be associated with breast enlargement.
Even though most cases of gynecomastia are diagnosed clinically, ultrasound plays an important role in differentiating a benign appearance from mastitis or abscess. Some authors have described the appearance of ultrasonography of neonatal mastitis as masses with mixed echotexture and internal vascularity or as poorly marginated hyperechoic breast tissue with hypervascularity(5,6,18). Mastitis can be differentiated from abscess due to the presence of increased peripheral vascular distribution that they saw around cystic breast lumps(5,6,19,20). In our case, ultrasound demonstrated bilateral retroareolar mammary glandular tissue with asymmetrical left-right dimensions, suggestive for gynecomastia.
In this case, we can consider a possible connection between the association of gynecomastia in which left breast enlargement overlapped with the initiation of desogestrel contraceptive therapy in the mother of an exclusively breastfed infant, but further studies are needed to establish the exact mechanism. Furthermore, the favorable outcome of our patient after the discontinuation of maternal hormone therapy without a specific treatment is similar to the data in the literature(2,11,17,21).
Conclusions
Breast enlargement in newborns is a common transient physiological condition that can occur in both girls and boys. It is important to distinguish newborn gynecomastia from mastitis or breast abscess. Parents should be informed that it will resolve in weeks to a few months, without treatment, and should be warned not to squeeze the breast. The most appropriate approach is to observe the breast involution. Further studies are needed to investigate the correlation between the use of progestogen (progestogen-only pill desogestrel) in breastfeeding mothers and the development of breast enlargement in breastfeeding infants.
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
-
Kaneda HJ, Mack J, Kasales CJ, Schetter S. Pediatric and adolescent breast masses: a review of pathophysiology, imaging, diagnosis, and treatment. AJR Am J Roentgenol. 2013;200(2):W204-W212.
-
Sevinç S, Almus E, Okulu E, et al. A Newborn with Bilateral Breast Enlargement: Neonatal Mastauxe. Journal of Ankara University Faculty of Medicine. 2020;73(3):312-314.
-
Sharonda AT. Gynecomastia in children and adolescents. UpToDate. 2021 [cited 2022 may 15. Available at: https://www.uptodate.com/contents/gynecomastia-in-children-and-adolescents?search=Gynecomastia%20&source=search_result&selectedTitle=2~150&usage_type=default&display_rank=2.
-
Madlon-Kay DJ. “Witch’s Milk”. Galactorrhea in the Newborn. Am J Dis Child. 1986 March; 140(3).
-
Suthar B, Aggarwal K. A rare case of neonatal mastauxe: Case report. Indian J Radiol Imaging. 2019;29(1):89-93.
-
Borders H, Mychaliska G, Gebarski KS. Sonographic features of neonatal mastitis and breast abscess. Pediatr Radiol. 2009;39(9):955-958.
-
Al Jurayyan NAM. Childhood Gynecomastia: A Mini Review. International Journal of Clinical Endocrinology and Metabolism. 2016 Jul; 2(1):012-015.
-
Jayasinghe Y, Cha R, Horn-Ommen J, O’Brien P, Simmons PS. Establishment of normative data for the amount of breast tissue present in healthy children up to two years of age. J Pediatr Adolesc Gynecol. 2010;23(5):305-311.
-
Trotter A, Maier L, Kohn T, Böhm W, Pohlandt F. Growth of the uterus and mammary glands and vaginal cytologic features in extremely premature infants with postnatal replacement of estradiol and progesterone. Am J Obstet Gynecol. 2002;186(2):184-188.
-
Raveenthiran V. Neonatal mastauxe (breast enlargement of the newborn). J Neonatal Surg. 2013;2(3):31.
-
Phillips SJ, Tepper NK, Kapp N, Nanda K, Temmerman M, Curtis KM. Progestogen-only contraceptive use among breastfeeding women: a systematic review. Contraception. 2016;94(3):226-252.
-
Truitt ST, Fraser AB, Grimes DA, Gallo MF, Schulz KF. Hormonal contraception during lactation: systematic review of randomized controlled trials. Contraception. 2003;68(4):233-238.
-
Progestogen-only contraceptives during lactation: II. Infant development. World Health Organization, Task Force for Epidemiological Research on Reproductive Health; Special Programme of Research, Development, and Research Training in Human Reproduction. Contraception. 1994;50(1):55-68.
-
Halderman LD, Nelson AL. Impact of early postpartum administration of progestin-only hormonal contraceptives compared with nonhormonal contraceptives on short-term breast-feeding patterns. Am J Obstet Gynecol. 2002;186(6):1250-1258.
-
Tepper NK, Phillips SJ, Kapp N, Gaffield ME, Curtis KM. Combined hormonal contraceptive use among breastfeeding women: an updated systematic review. Contraception. 2016;94(3):262-274.
-
Effects of hormonal contraceptives on breast milk composition and infant growth. World Health Organization (WHO) Task Force on Oral Contraceptives. Stud Fam Plann. 1988;19(6 Pt 1):361-369.
-
Bjarnadóttir RI, Gottfredsdóttir H, Sigurdardóttir K, Geirsson RT, Dieben TO. Comparative study of the effects of a progestogen-only pill containing desogestrel and an intrauterine contraceptive device in lactating women. BJOG. 2001;108(11):1174-1180.
-
Kachewar S, Kachewar S. Sonomammography in Neonatal Mastauxe. Cukurova Medical Journal. 2015;40:22-24.
-
Kurtoğlu S, Direk G, Tatlı ZU, Hatipoğlu N. Transient endocrinologic problems in the newborn period. Turk Pediatri Ars. 2019;54(1):3-12.
-
Kaufman J, Messazos B, Sharples-Blissland N, Cameron F. Extreme physiological gynaecomastia in the neonate: Observation not intervention. J Paediatr Child Health. 2015;51(10):1030-1032.
-
Amer A, Fischer H. Neonatal Breast Enlargement. The New England Journal of Medicine. 2009 Apr; 360(14):1445.