Opioids are commonly prescribed by oncology and palliative care physicians, with the intent of relieving suffering related to cancer pain. However, these medications have multiple side effects, opioid-induced constipation (OIC) being one of the most common adverse effects encountered in clinical practice. Several tools can be used to diagnose OIC, but asking patients about changes in bowel habits since starting opioids is essential, otherwise OIC may go undiagnosed. Multiple medications, briefly reviewed in this article, such as laxatives, peripherally acting mu-opioid receptor antagonists, chloride channel activators, or guanylate cyclase-C receptor agonists, can be used to treat OIC once it occurs, but prevention is essential for the patient’s well-being and compliance with opioid therapy.
Constipaţia indusă de opioide
Opioid-induced constipation
First published: 16 mai 2018
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/OnHe.43.2.2018.1693
Abstract
Rezumat
Opioidele, prescrise de medicii oncologi şi de cei de îngrijire paliativă pentru uşurarea durerii din cancer, au efecte secundare multiple, constipaţia fiind unul dintre cele mai frecvente. Constipaţia produsă de opioide poate să rămână nediagnosticată dacă pacientul nu este întrebat despre orice schimbare apărută în funcţionalitatea tractului digestiv după începerea terapiei cu opioide. Prevenirea constipaţiei este esenţială pentru bunăstarea pacientului şi pentru succesul tratamentului cu opioide. Constipaţia poate fi tratată cu diferite medicamente, cum sunt laxativele, antagoniştii periferici ai receptorului opioid mu, activatorii canalelor de clor sau agoniştii receptorilor guanilat-ciclazei-C, descrise în acest articol.
Opioids are essential drugs in relieving suffering from pain in the cancer population. Unfortunately, these drugs have significant side effects, including constipation, nausea and vomiting, pruritus, respiratory depression, opioid-induced neurotoxicity and opioid-induced hypogonadism, as well as the possibility of accidental overdose and death.
Opioid-induced constipation (OIC), the most common side effect of opioids, may adversely affect one’s quality of life and work productivity, and can also explain why about a third of patients end up reducing or discontinuing opioid medications altogether in an attempt to improve bowel function(1).
Constipation is defined by the Rome IV criteria as two or more of the following symptoms present for at least three months prior to the diagnosis:
1. Straining in more than 25% of defecations.
2. Hard lumpy stools (looking like nuts) or lumpy sausage shaped (Bristol Stool Form Scale 1 and 2) in more than 25% of defecations.
3. Sensation of incomplete evacuation in more than 25% of defecations.
4. Sensation of anorectal obstruction or blockage in more than 25% of defecations.
5. Manual manoeuvres to facilitate evacuation in more than 25% of defecations.
6. Fewer than three spontaneous bowel movements per week.
7. Loose stools are rarely present without the use of laxatives.
8. Insufficient criteria to diagnose irritable bowel syndrome with predominant constipation or mixed bowel habits(2).
OIC can occur days to weeks after the initiation of opioids, may get worse after changing or increasing the opioid dose, and persists even after the patient develops opioid tolerance. OIC may be less intense with transdermal fentanyl or methadone(2,3).
Several studies have shown that OIC may be more common or more severe in the following circumstances:
1. Female gender.
2. Higher level of education.
3. Moderate to severe psychosocial impairment (i.e., depression, anxiety, impulsivity, labile mood, angry) or on antidepressant therapy (TCAs etc.).
4. Unemployed or disabled because of health-related problems(4).
5. Cancer diagnosis treated with taxanes, Vinca alkaloids, thalidomide or bortezomib.
6. Lack of privacy, such as the inpatient setting.
7. Sedentary lifestyle.
8. Decreased fluid or fiber intake.
The pathology of OIC appears to be secondary to delayed gastrointestinal peristalsis and increased sphincter tone caused by opioid stimulation of the mu and delta receptors found in the enteric nervous system (ENS). This triggers decreased gastrointestinal (GI) transit, with increased water resorption that in turn leads to hard stools and constipation(5).
The prevalence of OIC is high, though literature is not consistent regarding its frequency. A review article of 11 randomized studies about GI side effects from opioids showed that OIC was present in 41% of cases(2).
Another article suggested that OIC was present in 21% to 90% of the patients treated with opioids, with a prevalence depending on the type of the opioid, the duration of opioid usage, the presence of constipation prior to using opioids, and the use of other agents that could affect GI tract motility(5).
Other studies have shown that approximately 52% of the patients with advanced cancer suffer from constipation, this percentage being even higher in patients with cancer who are taking opioids (about 87%)(7).
However, despite being so common, OIC remains an underdiagnosed condition possibly due to prescribers’ lack of awareness on OIC, or due to failure to ask patients direct questions about it, or because of the patients’ embarrassment to report it(5).
The most common symptoms encountered by patients developing OIC are: bloating, heartburn, nausea, sometimes vomiting, decreased appetite, abdominal pain, and passing of hard stool with straining(5).
Several scales may be used to diagnose OIC, such as:
1. Bristol Stool Form Scale, which classifies the forms of feces into 7 groups, with types 1 and 2 (described above) representing constipation, types 3 and 4 being the normal, and types 5 to 7 representing diarrhea(5).
2. Bowel Function Index (BFI), a clinician-administered scale, rates the ease of defecation, bowel evacuation, and the patient’s judgement of the constipation over the past week. Each item is scored on a scale between 0 and 100, with scores less than 28 representing a normal bowel function(5).
3. Patient Assessment of Constipation Quality of Life (PAC-QOL) is a 28-item questionnaire assessing the burden of constipation on the patient’s everyday functioning by using a 5-point scale from 0 to 4. A score of 0 is considered normal(5,8).
4. Patient Assessment of Constipation Symptoms (PAC-SYM) is a 12-item questionnaire assessing the severity of constipation on a 5-point scale (from 0 to 4) in three domains: stools, abdominal symptoms and rectal symptoms, over the past two weeks. A score of 0 rules out the presence of constipation(8).
5. Constipation Assessment Scale (CAS) is a patient-administered questionnaire assessing the severity of multiple symptoms, such as: abdominal distension, flatus, frequency of bowel movements, consistency and volume of stools, presence of pain with defecation, and presence of rectal fullness or pressure. A score of 0 represents the normal, whereas a score of 16 is suggestive of severe constipation(9).
The diagnosis of OIC is made clinically, by interviewing the patient, and by physical examination, including a rectal exam if the white blood count (WBC) and platelet count permit.
Imaging studies, such as plain abdominal X-ray, can also help in the diagnosis of OIC, or be used to rule out the evidence of obstruction.
A useful tool is the constipation score obtained by assessing the content of stool on a plain abdominal X-ray divided into four quadrants, using a scale from 0 to 3, where 0 represents the absence of stool and 3 represents stool impaction. The maximum score is 12, and a score of 7 or above is suggestive for severe constipation, requiring aggressive management(10).
The treatment of OIC involves both non-pharmacological and pharmacological approaches. The non-pharmacological approach includes counseling patients to increase their fiber and fluid intake. Eating fruits like apples, prunes and bananas, or vegetables like string beans, spinach and peas, as well as avoiding constipating foods like dairy products can be helpful. However, it is recommended not to exceed 25-30 grams of fiber daily to avoid feeling bloated. Although physical exercise can raise serious challenges in patients with advanced cancer, it should also be encouraged whenever possible.
Sometimes a simple clockwise abdominal massage can bring some relief from OIC(5,11).
In severe cases, manual disimpaction may be helpful, provided that the patient does not have leukopenia and/or thrombocytopenia.
The pharmacological approach involves the use of laxatives, peripherally acting mu-receptors antagonists (PAMORAs) agents, chloride channel activators, guanylate cyclase-C receptor agonists, suppositories and enemas.
Guidelines provided by the European Society for Medical Oncology recommend that laxatives, presented in Table 1, should be routinely prescribed to prevent and treat OIC.
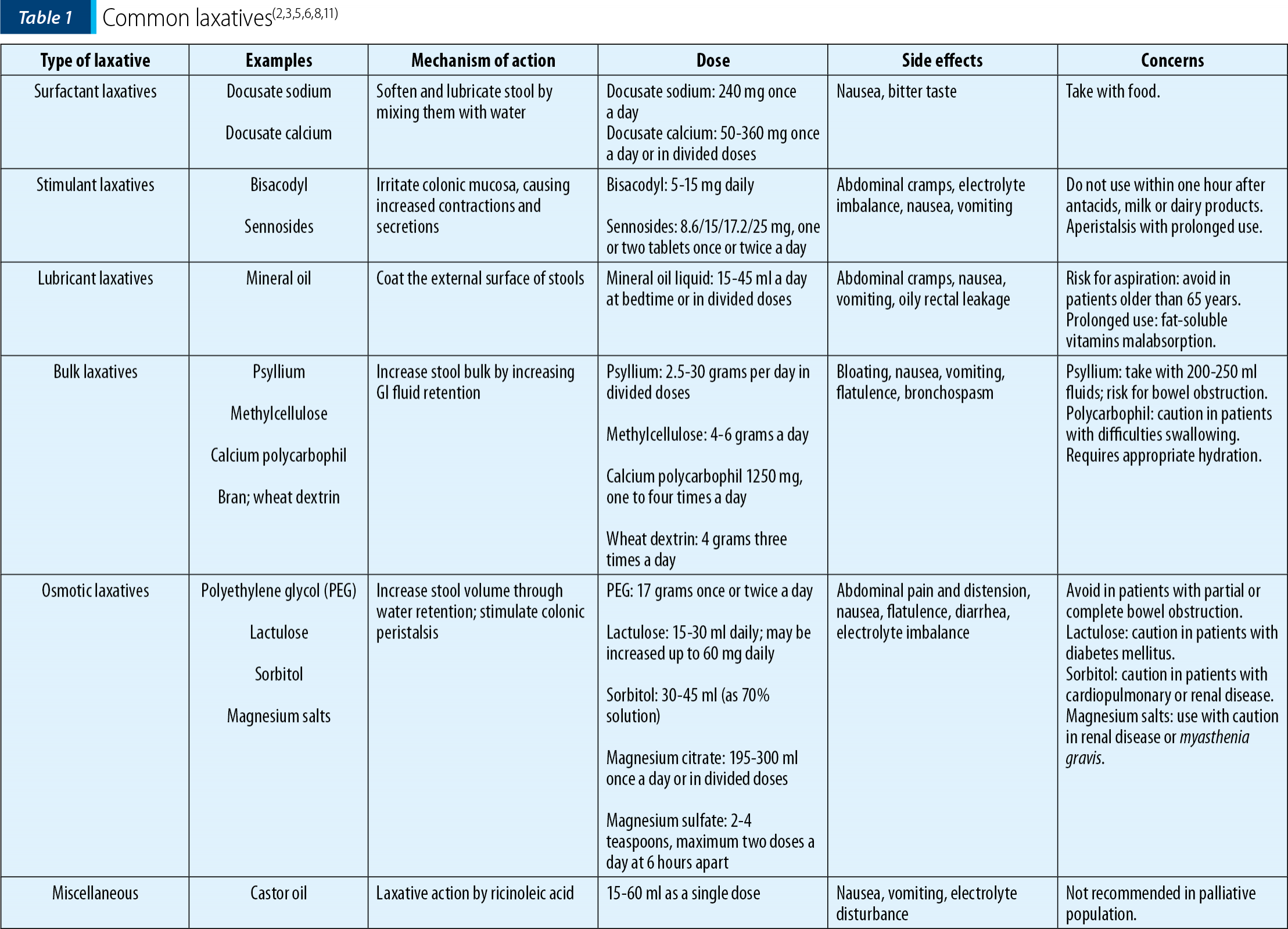
The European Consensus Group on Constipation recommends using a combination of osmotic and stimulant laxatives(8).
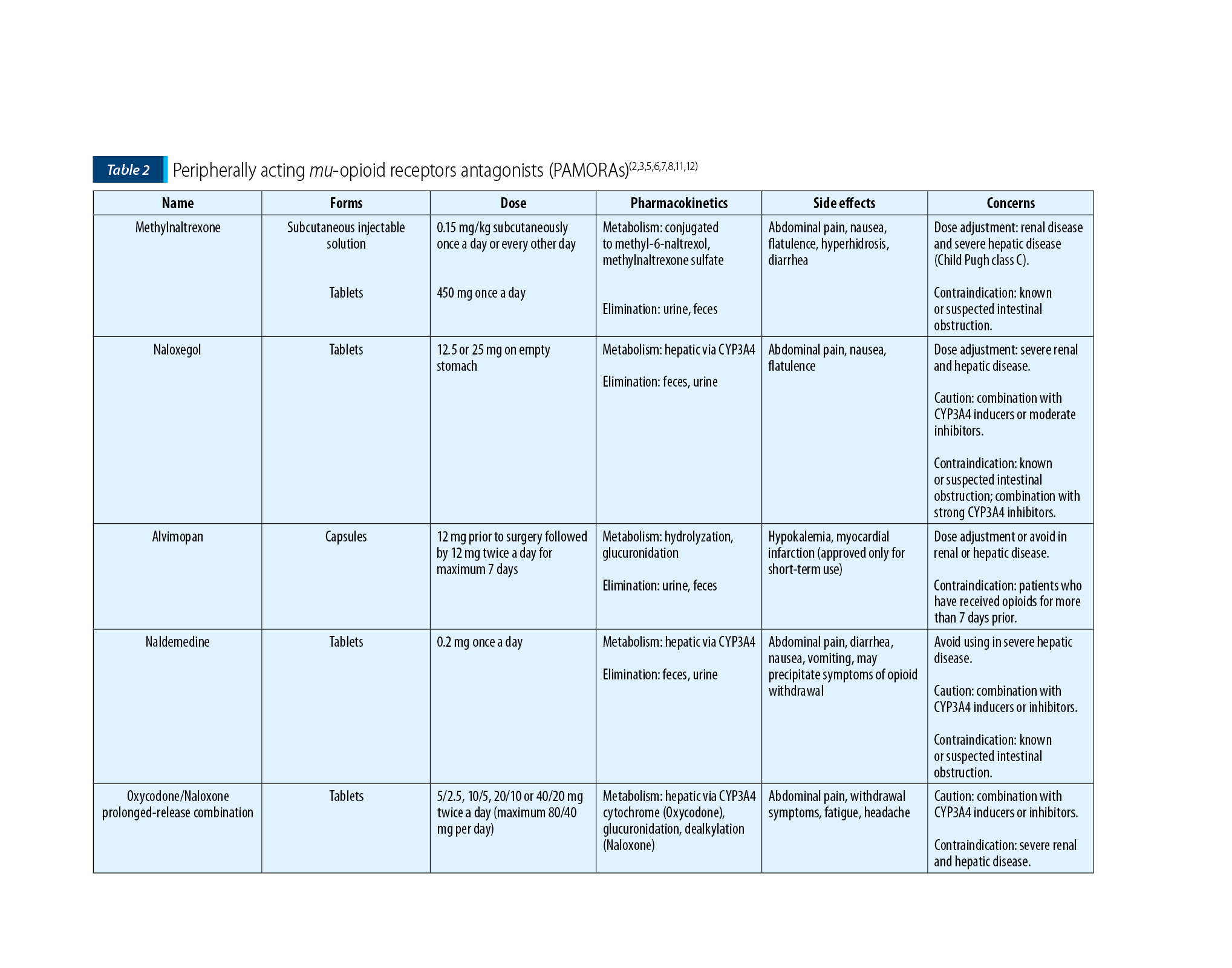
PAMORAs, listed in Table 2, act by blocking opioids from binding to the peripheral mu-opioid receptors located in the gut. It is generally accepted that they do not cross the blood-brain barrier to interfere with the analgesic effect of the opioids(3,6). However, caution is advised in patients who may have a disruption of the blood-brain barrier, such as primary or secondary cancers of the central nervous system (CNS) or after brain iradiation(7).
Chloride channel activators act by stimulating the chloride channels in the gut, thus increasing fluid secretion and fecal transit. Lubiprostone at a dose of 8 or 24 mcg twice a day does not interact with the cytochrome CYP3A4, which makes it an attractive option for patients on polypharmacy. Some studies have shown, however, that methadone may attenuate lubiprostone’s efficacy. This medication is contraindicated for patients with known or suspected bowel obstruction(3,5,11).
Guanylate cyclase-C receptor agonists, such as linaclotide at doses of 72, 145 or 290 mcg a day, plecanatide at 3 mg daily, and prucalopride, are approved for chronic idiopathic constipation and irritable bowel syndrome with constipation predominance. Prucalopride is available in Europe and Canada, but not yet in the USA.
The use of enemas should be reserved for the most severe cases of OIC, provided that the patient’s WBC and platelet count allow for such invasive procedures.
In conclusion, clinicians prescribing opioids for pain relief need to remember that OIC is one of the most frequent side effects and cannot be overlooked. Prevention is the best way to manage OIC, even though currently we have a plethora of drugs to treat it.
Abbreviations:
OIC = Opioid-Induced Constipation
ENS = Enteric Nervous System
GI = Gastrointestinal
BFI = Bowel Function Index
PAC-QOL = Patient Assessment of Constipation Quality of Life
PAC-SYM = Patient Assessment of Constipation Symptoms
CAS = Constipation Assessment Scale
WBC = White Blood Count
PAMORAs = Peripherally Acting Mu-Receptor Antagonists
PEG = Polyethylene Glycol
CNS = Central Nervous System
Conflict of interests: The authors declare no conflict of interests.
Bibliografie
- Nee J, Zakari M, Sugarman MA, Whelan J, Hirsch W, Sultan S, Ballou S, Iturrino J, Lembo A. Efficacy of Treatments for Opioid-Induced Constipation: A Systematic Review and Meta-Analysis. Clinical Gastroenterology and Hepatology. 2018; Jan 25. pii: S1542-3565(18)30087-9. doi: 10.1016/j.cgh.2018.01.021.
- Lee AA, Hasler WL. Opioids and GI Motility – Friend or Foe?. Current Treatment Options in Gastroenterology. 2016; Dec;14(4):478-494.
- Murphy JA, Sheridan EA. Evidence-Based Review of Pharmacotherapy for Opioid-Induced Constipation in Non-Cancer Pain. Annals of Pharmacotherapy. 2018; Apr; 52(4):370-379. doi: 10.1177/1060028017739637. Epub 2017 Nov 2.
- Bhimji SS, Burns B. Narcotic Bowel Syndrome. StatPearls [Internet]. 2018; Treasure Island (FL): StatPearls Publishing; Apr 5.
- Bhimji SS, Witten RA. Constipation, opioid induced. StatPearls [Internet]. 2018; Treasure Island (FL): StatPearls Publishing; Mar 24.
- Streicher JM, Bilsky EJ. Peripherally acting mu-opioid receptor antagonists for the treatment of opioid-related side effects: mechanism of action and implications. Journal of Pharmacy Practice. 2017; Jan 1:897190017732263. doi: 10.1177/0897190017732263
- Boland JW, Boland EG. Pharmacological therapies for opioid-induced constipation in adults with cancer. BMJ. 2017; Aug 2; 358: j3313. doi: 10.1136/bmj. j3313.
- Garcia JM, Shamliyan TA. Management of Opioid-Induced Constipation in Patients with Malignancy. American Journal of Medicine. 2018; Apr 2. pii: S0002-9343(18)30292-4. doi: 10.1016/j.amjmed.2018.02.038.
- McMillan SC, Williams FA. Validity and reliability of the Constipation Assessment Scale. Cancer Nursing. 1989; Jun; 12(3):183-8.
- Nagaviroj K, Yong WC, Fassbender K, Zhu G, Oneschuk D. Comparison of the Constipation Assessment Scale and Plain Abdominal Radiography in the Assessment of Constipation in Advanced Cancer Patients. Journal of Pain and Symptom Management. 2011; Aug; 42(2):222-8. doi: 10.1016/j.jpainsymman.2010.11.019. Epub 2011 Mar 31.
- Bowers BL, Crannage AJ. The Evolving Role of Long-Term Pharmacotherapy for Opioid-Induced Constipation in Patients Being Treated for Noncancer Pain. Journal of Pharmacy Practice. 2017; Jan 1:897190017745395. doi: 10.1177/0897190017745395.
- Burness CB, Keating GM. Oxycodone/Naloxone prolonged-release: a review of its use in the management of chronic pain while counteracting opioid-induced constipation. Drugs. 2014; Mar; 74(3):353-75. doi: 10.1007/s40265-014-0177-9.