Introduction. We chose colon cancer as a subject of our study because, beyond the screening efforts and of a minimally invasive precision surgery, supported by the latest generation oncology therapies, adapted to genetic analysis and the calculation of the individual risk of patients, we are still confronting with a low survival prognosis, which correlates with lymph node status. Unlike rectal cancer, to which the surgical treatment has moved to the secondary plane, surgery remains the saving therapeutic solution for colon cancer. Several recent studies analyzing neoadjuvant immunotherapy are ongoing but require further evaluations to demonstrate the long-term benefit. Materials and methods. We performed a literature search in the PubMed database from the last five years using the words of interest, as follows: current affairs, colon cancer, surgical treatment, transanal, extensive lymphadenectomy, sentinel lymph node. In addition, papers from the reference bibliography were consulted. Results. The main topics of scientific debate individualized in recent years converge towards a personalized surgery to optimize colonic resection and radicality by extending lymphadenectomy, by intraoperative evaluation of colon vascularization, as well as by lymphatic drainage mapping and guiding colon resections according to local anatomical peculiarities. Our search generated 402 titles, of which 89 in the last year. Subsequently, those that did not have the abstract available or were not written in English were excluded. Discussion. Recent studies have observed that the efforts to detect micrometastases, as well as the extensive excision of the regional ganglia confered a more precise pathological anatomy staging and improved the oncological prognosis of the patient. Conclusions. Current technologies, both in terms of diagnosis and treatment, allow us to perform an extensive radical surgery with minimal risks in the short and long term.
Current strategy and future directions in colon cancer surgery – literature review
Strategia actuală şi direcţii viitoare în chirurgia cancerului de colon. Review al literaturii
First published: 31 mai 2023
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/OnHe.63.2.2023.8089
Abstract
Rezumat
Introducere. Am ales ca subiect de studiu cancerul de colon pentru că, dincolo de eforturile de screening şi ale unei chirurgii de precizie minim invazivă, susţinute de terapiile oncologice de ultimă generaţie, adaptate la analiza genetică şi calcularea riscului individual al pacienţilor, ne confruntăm în continuare cu un prognostic de supravieţuire redus, care se corelează cu invazia limfoganglionară. Spre deosebire de cancerul rectal, la care tratamentul chirurgical a trecut în plan secundar, chirurgia rămâne soluţia terapeutică salvatoare pentru cancerului de colon. Unele studii recente care analizează imunoterapia neoadjuvantă sunt în desfăşurare, dar necesită evaluări ulterioare pentru a demonstra beneficiul pe termen îndelungat. Materiale şi metodă. Am consultat literatura de specialitate din baza de date PubMed din ultimii cinci ani, folosind următoarele cuvinte-cheie: actualităţi, cancer de colon, tratament chirurgical, transanal, limfadenectomie extinsă, ganglion-santinelă. În plus, au fost consultate lucrări din bibliografia de referinţă. Rezultate. Principalele teme de dezbatere ştiinţifică individualizate în ultimii ani converg către o intervenţie chirurgicală personalizată pentru optimizarea rezecţiilor şi radicalităţii colonice, prin extinderea limfadenectomiei, prin evaluarea intraoperatorie a vascularizării colonului, precum şi prin cartografierea drenajului limfatic şi ghidarea rezecţiilor colonice în funcţie de particularităţile anatomice locale. Căutarea noastră a generat 402 titluri, dintre care 89 în ultimul an. Ulterior au fost excluse cele care nu aveau rezumatul disponibil sau care nu erau scrise în limba engleză. Discuţie. Studiile recente au observat că eforturile de decelare a micrometastazelor, cât şi excizia extinsă a ganglionilor regionali conferă o stadializare anatomopatologică mai precisă şi îmbunătăţeşte prognosticul oncologic al pacienţilor. Concluzii. Tehnologiile actuale, atât în ceea ce priveşte diagnosticul, cât şi tratamentul, ne permit să efectuăm o chirurgie radicală extinsă, cu riscuri minime pe termen scurt şi lung.
Introduction
Colon cancer is silent in the early stages and this involved an effort to mobilize medical resources for screening, but also for early diagnosis and treatment. The implementation in practice of the national screening programs in recent years has achieved its objectives, which are statistically reflected in terms of rising the incidence by increasing the early diagnosis of colorectal cancer. It ranked first in Romania according to GLOBOCAN 2020 reports for both sexes, on the third place in terms of incidence in males, after lung and prostate cancer, and on the second place in females, after breast cancer(1). Currently, due to changes in lifestyle and diet, the incidence has increased also among the young population, no longer being considered a cancer specific to the age of over 60 years old(2). Although important technological advances have been made in the treatment of colon cancer and minimally invasive surgical techniques have almost replaced open surgery, the prognosis is still reserved, being the second leading cause of death by cancer in Romania, after the localized pulmonary one, according to World Health Organization (WHO)(3). Worldwide artificial intelligence is already successfully used in diagnosing cancer and in analyzing the risk of preoperative complications(4,5).
The multimodal treatment of colon cancer, although discussed jointly in the guidelines with that of rectal cancer, differs in therapeutic attitude, the first intention being surgery, and a separation of guidelines has been discussed by specialists in the field(6). Colon cancer surgery may have a radical or palliative target, the decision being taken in the oncology committee at the time of the diagnosis of certainty anatomic pathology report (APR) correlated with paraclinical investigations and in accordance with TNM staging (AJCC)(7). Subsequently, the opportunity of chemotherapy or adjuvant immunotherapy will be reassessed after the surgery, depending on the biological and genetic profile of the tumor. Approximately 35% of colorectal cancers occur in family hereditary syndromes(8,9), the mechanisms being incompletely known, which is why genetic tests to identify MSI (microsatellite instability) and MMR (DNA mismatch repair) are recommended in patients with a family history of colorectal cancer(10,11). Testing for RAS mutations (KRAS, NRAS) and BRAF mutation, MLH 1, as well as chromosomal instability will guide the oncological treatment according to the molecular profile of the tumor(8,9).
The diagnosis of early colon cancer in the stage of malignant polyps allowed the performance of endoscopic polypectomies, mucosal and submucosal resections, with a curative visa, but also the association of laparoscopy to endoscopic resections (CELS – Combined Endoscopic-Laparoscopic Surgery) for a more efficient control of potential complications, with favorable results(12). Simultaneously with the development of submucosal dissection techniques, new techniques of closing the wide defects of mucosa with clips and even endoscopic suturing (Through-the-Scope-Suturing – TTSS) have been developed(13). Moreover, endoscopic robots were implemented in current routine surgery, minimizing the difficulty of approaches: Anubiscope, Endomaster, Flex robotic system(14). However, we cannot say the same about the rate of complications in open and laparoscopic surgery, which still remains at an increased level, surprisingly similar for both types of approach(15,16). The attention of the studies was channeled towards the detection of other factors of influence of the postoperative results, independent of the technique – for example, the perioperative biological status of the patient. Guidelines have been developed and many clinics in the world have adopted at hospital level protocols such as Enhanced Recovery After Surgery (ERAS)(17), with encouraging results.
Radical surgery of colon cancer involves the removal of the tumor en bloc with the colonic segment afferent to the main arterial pedicle, the mesocolon and the efferent lymphatic drainage, the primary ligation of the vascular pedicles being recommended(18).
Beyond the esthetic benefits and the much faster recovery of the patient that allows a rapid reintegration into society, minimally invasive surgery has not proven its superiority over open surgery in terms of oncological results. Regarding transanal surgery(19) in colon cancer, there are few data in the literature, only case studies at the moment, but the approach path is more often used successfully for the extraction of parts in laparoscopic or robotic surgery, NOSE technique(20), according to the same principle as NOTES (Natural Orifice Transluminal Endoscopic Surgery)(21), but more physiological.
This review of the literature aims to provide an overview of the therapeutic options in colon cancer at the moment and to bring into discussion the latest advances in the surgical field.
Materials and method
A literature search from the PubMed database in the last five years was consulted, from January 2018 to November 2022, using the words of interest as follows: advances colon cancer surgery, update, surgical treatment, sentinel lymph node, transanal surgery, D3 lymphadenectomy. In addition, there were consulted papers from the reference bibliography. The main topics of scientific debate individuated in recent years converge towards a personalized surgery for optimizing colonic resections and radicality by extending lymphadenectomy, by intraoperative evaluation of colon vascularization, as well as lymphatic drainage mapping and guiding colonic resections according to local anatomical peculiarities.
Results
Our search yielded 402 titles, of which 89 in the last year. Among these, there were excluded those that did not have the available summary or were not written in English. In the end, there were 68 systematic reviews, 52 meta-analyses, 90 clinical trials and 66 randomized clinical trials. Subsequently, those that discuss the surgical treatment of colon cancer were selected, excluding those related strictly to rectal cancer. Also, the bibliography of the reference articles was consulted.
Discussion
The surgical interventions accepted with the radical target for colon cancer are: right hemicolectomy, extended right hemicolectomy, transversectomy, high (intermediate) left segmental colectomy, extended left hemicolectomy, left hemicolectomy, low left segmental colectomy, subtotal colectomy and total colectomy, when performed by the principles of oncological surgery.
Endoscopic polypectomy proved to be sufficient for an excision within oncological limits in the case of incipient malignant tumors T1 at the level of adenomatous polyps(12), and although the safety margin was a topic of debate, at present, it is accepted at least 2 mm as sufficient to reduce the risk of tumor backlog. Other oncological considerations in the case of malignant polyps are the invasion of the submucosa which can be of three degrees, superficial, intermediate and deep, and which has been shown to correlate directly proportionally with the increase in the risk of lymph node metastasis. A classification of pediculated polyps by Haggit(22) and of those sessile according to Kikuci(23) is mandatory and will direct the treatment to an eventual oncological resection when the risk of lymphatic metastasis is increased.
An increased attention should be paid to the detection of synchronous tumors, their incidence in the literature being estimated at 4-5% of colon cancers, explainable if we think about the precursor lesions which are often multiple. Depending on the location but also on the precursor lesion, the surgical treatment may consist of two colon segmental resections or subtotal colectomy, increasing the postoperative morbidity and decreasing the quality of life. Certain localizations are more problematic and there are debates about transverse colon cancer, especially those located at the splenic angle(24). They refer to the segmental transverse colectomy versus the extended right or left colectomy because studies have shown that wide organ excision is associated with a low survival. Also, on the same topic, an Italian study conducted in 2020(25) revealed that segmental resections have a lower rate of postoperative complications and an increase in survival to three years. Although there is a small possibility of metastasis in the lymphatic drainage area of the superior mesenteric artery estimated up to 9%(16) in cancers located at the splenic angle, the extension of the colectomy is not justified, except in isolated cases. The sentinel lymph node dissection would be useful in such situations for case selection.
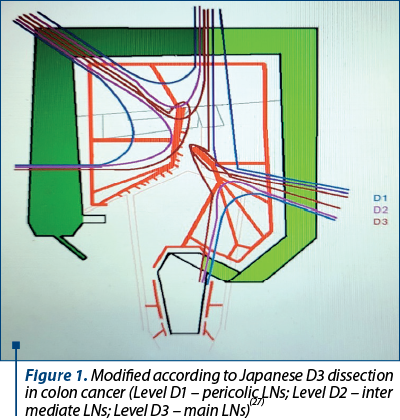
There is an ongoing study, called T-REX(26) prospective observational cohort, that includes 4000 patients from 35 participating institutions in Japan, South Korea, Germany, Russia, Lithuania and Taiwan, that analyzes lymphadenectomy in colon cancer on three levels of radicality: A(26) (it raises the lymph nodes up to the middle of the colic artery), B (it also raises the ganglia from the origin of the colic artery without exposure of the upper mesenteric artery and vein in the case of the right colon, and is subclassified in B1 up to the origin of the sigmoid trunk, respectively B2, the origin of the left colic artery), C (it excises the ganglia around the upper artery and mesenteric vein C1 to the left of the superior mesenteric vein, C2 to the left of the superior mesenteric artery, and C at the origin of the inferior mesenteric artery for the left colon). This should be applied to any of the four colonic regions depending on the main vascular pedicle, namely: the ileocolic artery/right colic, the middle colic artery, the left colic artery, and the trunk of the sigmoid arteries(27). It aims to elucidate lymph node (LN) metastasis in colon cancer and to issue an international standardization of the regional ganglia in colon cancer, but also of the optimal colonic resection depending on the location of the tumors and on the vicinity of the vascular pedicle, as there is no standardization of radical colectomy at the international level.
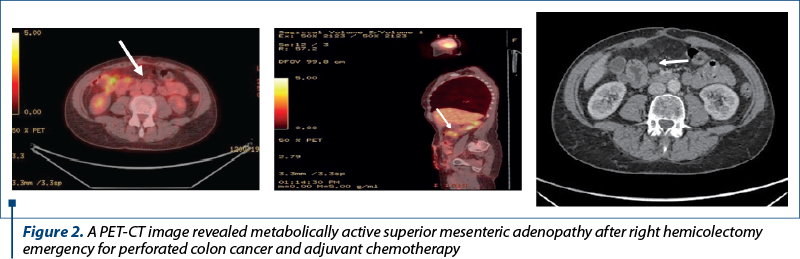
New studies are underway to support extensive lymphadenectomy especially in colon cancer, as similar to total excision of mesorectum in rectal cancer. The desiderata of a type D3 lymphadenectomy in colon cancer according to the Japanese treatment guidelines (JSCCR)(27) (Figure 1) imply a complete dissection and excision of the regional ganglia. The criteria of radicality in the D3 lymphadenectomy of the right colon (Figures 2) imply, in addition to the complete excision of the mesocolon, first described by W. Hohenberger in 2009(28), by dissection in embryological planes with high ligation of the right colic vessels (CVL – central vascular ligation), a Gillot surgical trunk dissection(29) of the superior mesenteric vein and dissection in the region of the venous trunk of Henle. Ligation of the Henle trunk at the origin is recommended to be avoided as much as possible by preferring separate ligation of the right colic vein(26). It has not yet been decided to adopt it as a standard or routine in colon surgery, but there are studies that show a better staging of the lymph nodes by using this technique(30-32). Others, however, do not support this idea and declare that no improvement in survival has been observed; on the contrary, it would increase the rate of complications such as gastric stasis through a delayed emptying(33) associated with lymph node dissection of the gastrocolic ligament, or by the appearance of postoperative diarrhea due to damage to the upper mesenteric artery plexus (SMAP) during lymph node dissection(34).
The personalized surgery depending on the anatomical variants of vascularization and the length of the colon, the location of the tumor, as well as the stage of the disease made it difficult to standardize the technique and also analyze the results(35-37). However, studies are underway to compare standard lymphadenectomy with intermediate and extended lymphadenectomy, the analysis criteria including also well-defined histopathological assessment of anatomical margins in the resected specimen.
Chen et al.(38) practiced the laparoscopic 3D approach to increase the accuracy of D3 lymph node dissection in colon cancer, under the control of visualizing arterial anatomical variants and also compared preoperative CT guidance with real-time, without noticing differences between the two groups in terms of duration of surgery, blood loss, vascular lesions or the number of extirpated lymph nodes. Thus, a preoperative 3D reconstruction seems to be enough to avoid major complications.
The sentinel lymph node technique in colon cancer(39-41) is not performed routinely, but studies have proven its usefulness in spotting potential ganglia with micrometastases, increasing the number of harvested lymph nodes and, implicitly, providing a more accurate diagnosis, increasing the patient’s chances of benefiting from adjuvant treatment that in other conditions he would not receive. Also, the use of a new solution for solving tissue around ganglia (Carnoy’s solution) improved the count of more ganglia compared to conventional histopathological specimen examination(42).
Neoadjuvant chemoradiotherapy treatment proved effective only in patients with T4b tumors by increasing with 23% the survival without the disease, compared to patients who benefited only from adjuvant treatment. Thus, neoadjuvant chemoradiation therapy is currently used only in isolated cases after analysis in the multidisciplinary commission, for patients with locally advanced sigmoid colon cancer (LASCC). Two reference clinical trials (FOxTROT(43) and PRODIGE 22(44)) analyzed the results obtained with neoadjuvant therapy in patients with colon cancer. There were no improvement in terms of overall survival or without disease compared to those obtained by adjuvant treatment. The morbidity and mortality recorded were similar between the two treatment groups. Neoadjuvant immunotherapy(45) in selected cases of early colon cancer followed by radical surgery led to obtaining a complete histopathological response on the resection piece in a high percentage of cases and to a partial response in all cases which makes it a potential candidate as a standard of treatment in selected cases correlated with MMR status. Thus, it is disputed the primacy of surgery in these patients.
Regarding the minimally invasive surgical approach(46-48) or opened, multiple randomized international studies have shown similar results in terms of compliance with oncological standards and, in addition, a decrease in hospitalization, with the mention that the analysis was done in centers of excellence, where surgeons are experienced and familiar with the technique and that the results may vary during the learning curve of the technique. Regarding robotic surgery(49), the only disadvantages described were the increased operating time and the unjustified costs, as long as the oncological results do not prove superior and do not worth the investment of resources.
Regarding the radial extension and the invasion or adherence to the organs in the vicinity of the tumor, new studies carried out recommend the block excision of the organs to which the tumor adheres, and do not recommend adhesiolysis at this level because, in a percentage of 34% to 84% of cases, tumor infiltrated at the microscopic level was proven(50).
New therapeutic solutions for stenosis colon cancer – limits and oncological safety
New treatment solutions have been implemented in the current practice of obstructive advanced colon cancer, and the oncological treatment guidelines propose self-expandable metal stents, first described by Dohomoto in 1991(51), as an alternative to colostomy or segmental resections with colostomy, especially for cancers located in the left colon(52) and less often for cancers of the right colon. Although initially the technique was used with the palliative visa, more and more studies have reported favorable results in the use of the technique as a preamble (BTS – “bridge to surgery”) of elective surgery with radical visa. The advantages are multiple and we mention that it does not require a long recovery such as performing a colostomy(53,54), thus allowing a faster access to neoadjuvant treatment. Various studies have shown similar results in five-year survival and the overall survival of the two-stoma versus stent therapeutic groups, without compromising the oncological safety of patients. Another benefit of using metal stents mentioned in the studies carried out in patients with colon cancer in non-metastatic stage consisted in facilitating the performance of an anastomosis per primam, when it was performed for curative purposes, with the reduction of morbidity and mortality to 30 days(55). Colon stenting proved to be a successful alternative therapy that allowed anastomoses to be performed without the protection of an ileostomy, thus avoiding nutritional imbalances. However, further studies are necessary to prove the oncological safety and the introduction of the method as a therapeutic standard, as well as to establish the optimal moment of the surgical intervention(56) with the radical visa, in relation to the insertion of the metallic stent.
In a study conducted in South Korea, which also proposed to analyze the oncological safety of patients with colon cancer with different therapeutic approaches, perineural invasion was comparatively analyzed in patients operated laparoscopically after stent placement and in those in whom colectomy was performed in an emergency per primam. The rate of perineural invasion of the primary tumor was significantly higher (76% versus 51.4%; p=0.033) than that of the patients operated in emergency, the surprising fact being that this did not influence the survival at five years or the survival without disease at five years, these being similar(57,58). It is estimated a perforation rate of 2% to 9% and, implicitly, associated with locoregional relapse in these patients(16). When septic complications occur, abscess or peritonitis, oncological resection is recommended and, of course, it changes the short- and long-term prognosis of the patient. There are no studies in the literature that analyze bleeding as a post-endoscopic stent related complication of colon tumors, nor how frequently it occurs; we found a single case presentation article that relates the migration of a stent with colonic-arterial external iliac fistula(59,60).
In the metastatic stage(61,62), when liver or lung tumors can be surgically sanctioned, their excision is required because it has proven useful in increasing survival in patients with stage IV colon cancer. The decision to address the colon tumor and liver metastases concomitantly or successively will be adapted on a case-by-case basis and discussed in the oncology committee. A higher percentage of survival without disease progression by up to 7% or more was recorded in the case of neoadjuvant chemotherapy, according to the EORCT 40983 study(63). The pulmonary metastasectomies, when performed, did not alter the overall median survival, being the same in both groups, 3.5 and 3.8 years, respectively(16).
The approach to peritoneal metastases was evaluated in a randomized multicenter study in 2021, PRODIGE-7(64), and the results revealed higher rates of adverse complications in cases where HIPEC(65) was associated with cytoreduction, without improving the overall survival, which reduced the enthusiasm of specialists for this therapeutic approach, however difficult to access due to the special conditions required to perform it from a technical point of view, not accessible on a large scale. Better results are reported with the new technique of pressurized intraperitoneal aerosol chemotherapy (PIPAC)(66,67).
While the treatment of colon cancer seems to be almost standardized and the results predictable, in the Italian research, questions arise regarding the accuracy of the stadialysis(68,69), in the sense that the studies carried out have reported under-appreciations of the locoregional extension, which negatively influences the treatment of patients, depriving them of the chance of neoadjuvant chemotherapies. So, perhaps special attention is required here to find a way to improve diagnosis – why not – by training and standardizing the information at the level of the institution with the international ones in real time. We must look for the cause of the unfavorable results and improve the clinical and paraclinical evaluation. We have high-performance equipment, we have advanced surgical therapies and techniques, and maybe it is appropriate to invest for the training specialists to exploit the equipment at its maximum potential. Medicine is evolving rapidly and, until the robotization of the entire process, may be worth facilitating access to information to the specialists locally, at the level of the institution in which they operate. Telemedicine is a solution, but it is not the only one, and it does not replace interdisciplinary communication, anyway.
The need to improve the biological status of the patient should be looked at in perspective, knowing that most of the time surgery is followed by an adjuvant oncological treatment. Although 83% of American and European surgeons support the importance of evaluating and optimizing the perioperative nutritional status of patients(70,71), studies conducted in the U.S. and Europe regarding the implementation of ERAS-type protocols at the hospital level found their application for only 20% of patients who required oncological surgery in the digestive sphere. Moreover, it has been observed that only in one in five hospitals formal nutritional screening is applied, which reveals a discrepancy between the opinion of experts in the field of surgery and the management at the hospital level.
All these desiderata are more difficult to implement in emergency surgery(72) and find their usefulness rather at the level of oncological institute, where the patient is evaluated in the oncological committee from the moment of diagnosis. Subsequently, the patient is often scheduled for elective surgery, and less often in the emergency, the emergency surgery being necessary only for hemorrhagic or obstructive cases that do not allow timing.
Diminishing postoperative complications increases the patient’s chances of receiving adjuvant treatment on time.
Conclusions
1. The study we carried out highlighted that we switched from performing open to laparoscopic and robotic interventions with the same oncological results, but less invasive, with improved surgical times, the minimally invasive surgery not being inferior to open surgery.
2. The current oncological clinical trials have increased the survival of the patients by associating neoadjuvant and adjuvant treatments to the surgical treatment, and also with a satisfactory degree of the quality of life.
3. There are further studies reporting that an extended lymphadenectomy to D3 stations associated with the identification of new tumor markers and minimally invasive surgery may lead to enhance oncological clearance, and preoperative planning 3D models represent a promising tool when it comes to performing it in a safe way.

Conflict of interest: none declared
Financial support: none declared
This work is permanently accessible online free of charge and published under the CC-BY
Bibliografie
- https://gco.iarc.fr/today/home
- Siegel RL, Miller KD, Goding Sauer A, et al. Colorectal cancer statistics, 2020. CA Cancer J Clin. 2020;70(3):145-164. doi:10.3322/caac.21601.
- http://www.who.int/en/
- Wallace MB, Sharma P, Bhandari P, et al. Impact of Artificial Intelligence on Miss Rate of Colorectal Neoplasia. Gastroenterology. 2022;163(1):295-304.e5. doi:10.1053/j.gastro.2022.03.007.
- Mitsala A, Tsalikidis C, Pitiakoudis M, Simopoulos C, Tsaroucha AK. Artificial Intelligence in Colorectal Cancer Screening, Diagnosis and Treatment. A New Era. Curr Oncol. 2021 Apr 23;28(3):1581-1607. doi:10.3390/curroncol28030149.
- Salvatore L, Imperatori M, Arnoldi E, et al. Management of patients with early-stage colon cancer: guidelines of the Italian Medical Oncology Association. ESMO Open. 2020;5(6):e001001. doi:10.1136/esmoopen-2020-001001.
- Benson AB, Venook AP, Al-Hawary MM, et al. NCCN Guidelines Insights: Colon Cancer, Version 2.2018. J Natl Compr Canc Netw. 2018;16(4):359-369. doi:10.6004/jnccn.2018.0021.
- Montazeri Z, Li X, Nyiraneza C, et al. Systematic meta-analyses, field synopsis and global assessment of the evidence of genetic association studies in colorectal cancer. Gut. 2020 Aug;69(8):1460-1471. doi:10.1136/gutjnl-2019-319313.
- Shinji S, Yamada T, Matsuda A, et al. Recent Advances in the Treatment of Colorectal Cancer: A Review. J Nippon Med Sch. 2022;89(3):246-254. doi:10.1272/jnms.JNMS.2022_89-310.
- Hahn GD, Wetwittayakhlang P, Afif W, Bessissow T, Lakatos PL. Hereditary Nonpolyposis Colorectal Cancer in Association with Crohn’s Disease and Lynch Syndrome: The Importance of a Strict Endoscopic Surveillance. Case Rep Gastroenterol. 2022;16(1):116-121. doi:10.1159/000521919.
- Yen T, Stanich PP, Axell L, Patel SG. APC-Associated Polyposis Conditions. 1998 Dec 18 [updated 2022 May 12]. In: Adam MP, Everman DB, Mirzaa GM, Pagon RA, Wallace SE, Bean LJH, Gripp KW, Amemiya A, editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993–2023.
- Bulut M, Knuhtsen S, Holm FS, Eriksen JR, Gögenur I, Bremholm L. Combined endoscopic laparoscopic surgical treatment of advanced adenomas and early colon cancer. Dan Med J. 2019;66(8):A5562.
- Zhang LY, Bejjani M, Ghandour B, Khashab MA. Endoscopic through-the-scope suturing. VideoGIE. 2021;7(1):46-51. doi:10.1016/j.vgie.2021.08.006.
- Nakadate R, Iwasa T, Onogi S, et al. Surgical Robot for Intraluminal Access: An Ex Vivo Feasibility Study. Cyborg Bionic Syst. 2020;2020:8378025. doi:10.34133/2020/8378025.
- Rotermund C, Djinbachian R, Taghiakbari M, Enderle MD, Eickhoff A, von Renteln D. Recurrence rates after endoscopic resection of large colorectal polyps: A systematic review and meta-analysis. World J Gastroenterol. 2022;28(29):4007-4018. doi:10.3748/wjg.v28.i29.4007.
- Vogel JD, Felder SI, Bhama AR, et al. The American Society of Colon and Rectal Surgeons Clinical Practice Guidelines for the Management of Colon Cancer. Dis Colon Rectum. 2022;65(2):148-177. doi:10.1097/DCR.0000000000002323.
- Liu X, Wang Y, Fu Z. Impact of enhanced recovery after surgery on postoperative neutrophil-lymphocyte ratio in patients with colorectal cancer. J Int Med Res. 2020;48(6):300060520925941. doi:10.1177/0300060520925941.
- Tejedor P, Francis N, Jayne D, Hohenberger W, Khan J; on behalf the CME Project Working Group. Consensus statements on complete mesocolic excision for right-sided colon cancer-technical steps and training implications. Surg Endosc. 2022;36(8):5595-5601. doi:10.1007/s00464-021-08395-0.
- Huang L, Zhang X, Zeng Z, Hu H, Kang L. Pure transanal endoscopic colectomy for ascending colon cancer. Tech Coloproctol. 2020;24(11):1207-1211. doi:10.1007/s10151-020-02271-0.
- Sun P, Liu Z, Guan X, et al. Laparoscopic radical right hemicolectomy with transrectal-specimen extraction: a novel natural-orifice specimen-extraction procedure. Gastroenterol Rep (Oxf). 2020;9(2):182-184. doi:10.1093/gastro/goaa047.
- Gundogan E, Aktas A, Kayaalp C, Gonultas F, Sumer F. Two cases of laparoscopic total colectomy with natural orifice specimen extraction and review of the literature. Wideochir Inne Tech Maloinwazyjne. 2017;12(3):291-296. doi:10.5114/wiitm.2017.69227.
- Haggitt RC, Glotzbach RE, Soffer EE, Wruble LD. Prognostic factors in colorectal carcinomas arising in adenomas: implications for lesions removed by endoscopic polypectomy. Gastroenterology. 1985;89(2):328-36. doi:10.1016/0016-5085(85)90333-6.
- Kikuchi R, Takano M, Takagi K, Fujimoto N, Nozaki R, Fujiyoshi T, Uchida Y. Management of early invasive colorectal cancer. Risk of recurrence and clinical guidelines. Dis Colon Rectum. 1995;38(12):1286-95. doi:10.1007/BF02049154.
- Di Saverio S, Stasinos K, Stupalkowska W, et al. Long splenic flexure carcinoma requiring laparoscopic extended left hemicolectomy with CME and transverse-rectal anastomosis: technique for a modified partial Deloyers in 5 steps to achieve enough reach and preserving middle colic vessels. Langenbecks Arch Surg. 2022;407(1):421-428. doi:10.1007/s00423-021-02240-7.
- Milone M, Degiuli M, Allaix ME, et al. Mid-transverse colon cancer and extended versus transverse colectomy: Results of the Italian society of surgical oncology colorectal cancer network (SICO CCN) multicenter collaborative study. Eur J Surg Oncol. 2020;46(9):1683-1688. doi:10.1016/j.ejso.2020.01.006.
- Shiozawa M, Ueno H, Shiomi A, et al. Study protocol for an International Prospective Observational Cohort Study for Optimal Bowel Resection Extent and Central Radicality for Colon Cancer (T-REX study). Jpn J Clin Oncol. 2021;51(1):145-155. doi:10.1093/jjco/hyaa115.
- Hashiguchi Y, Muro K, Saito Y, et al. Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2019 for the treatment of colorectal cancer. Int J Clin Oncol. 2020;25(1):1-42. doi:10.1007/s10147-019-01485-z.
- Hohenberger W, Weber K, Matzel K, Papadopoulos T, Merkel S. Standardized surgery for colonic cancer: complete mesocolic excision and central ligation – technical notes and outcome. Colorectal Dis. 2009;11(4):354-64; discussion 364-5. doi:10.1111/j.1463-1318.2008.01735.x.
- Sun KK, Zhao H. Vascular anatomical variation in laparoscopic right hemicolectomy. Asian J Surg. 2020;43(1):9-12. doi:10.1016/j.asjsur.2019.03.013.
- Bertelsen CA, Kirkegaard-Klitbo A, Nielsen M, Leotta SM, Daisuke F, Gögenur I. Pattern of Colon Cancer Lymph Node Metastases in Patients Undergoing Central Mesocolic Lymph Node Excision: A Systematic Review. Dis Colon Rectum. 2016;59(12):1209-1221. doi:10.1097/DCR.0000000000000658.
- Fukuoka H, Fukunaga Y, Nagasaki T, et al. Lymph Node Mapping in Transverse Colon Cancer Treated Using Laparoscopic Colectomy with D3 Lymph Node Dissection. Dis Colon Rectum. 2022;65(3):340-352. doi:10.1097/DCR.0000000000002108.
- Palmeri M, Peri A, Pucci V, et al. Pattern of recurrence and survival after D2 right colectomy for cancer: is there place for a routine more extended lymphadenectomy? Updates Surg. 2022;74(4):1327-1335. doi:10.1007/s13304-022-01317-2.
- Deng Y, Huang S, Huang M, Wang X, Huang Y, Chi P. Gastrocolic ligament lymph-node dissection may increase the incidence of delayed gastric emptying after colon cancer surgery with D3 lymphadenectomy. Surg Today. 2021;51(6):897-905. doi:10.1007/s00595-020-02200-6.
- Luzon JA, Thorsen Y, Nogueira LP, et al. Reconstructing topography and extent of injury to the superior mesenteric artery plexus in right colectomy with extended D3 mesenterectomy: a composite multimodal 3-dimensional analysis. Surg Endosc. 2022;36(10):7607-7618. doi:10.1007/s00464-022-09200-2.
- Moen TM, Stimec B, Ignjatovic D. The Use of a Vascular Roadmap at Surgery Evens out Surgeons Expectations on Operating Time, Blood Loss, Lymph Nodes Harvest and Operative Difficulty when Performing Right Colectomy with Extended D3 Mesenterectomy. Chirurgia (Bucur). 2022;117(5):579-584. doi:10.21614/chirurgia.2766.
- Popescu RC, Botea F, Dumitru E, et al. Extended Lymphadenectomy for Proximal Transverse Colon Cancer: Is There a Place for Standardization? Medicine (Kaunas). 2022;58(5):596. doi:10.3390/medicina58050596.
- Kamshilin AA, Zaytsev VV, Lodygin AV, Kashchenko VA. Imaging photoplethysmography as an easy-to-use tool for monitoring changes in tissue blood perfusion during abdominal surgery. Sci Rep. 2022;12(1):1143. doi:10.1038/s41598-022-05080-7.
- Chen J, Yuan Y, Peng W, Tang Y, Chen X, Wang Y, Shen H, Li R. [Application of three-dimensional visualization technique in laparoscopic D3 radical resection of right colon cancer]. Nan Fang Yi Ke Da Xue Xue Bao. 2022;42(5):760-765. [Chinese] doi:10.12122/j.issn.1673-4254.2022.05.19.
- Stăniloaie D, Budin C, Vasile D, et al. Role of methylene blue in detecting the sentinel lymph node in colorectal cancer: In vivo vs. ex vivo technique. Exp Ther Med. 2022;23(1):72. doi:10.3892/etm.2021.10995.
- Burghgraef TA, Zweep AL, Sikkenk DJ, van der Pas MHGM, Verheijen PM, Consten ECJ. In vivo sentinel lymph node identification using fluorescent tracer imaging in colon cancer: A systematic review and meta-analysis. Crit Rev Oncol Hematol. 2021;158:103149. doi:10.1016/j.critrevonc.2020.103149.
- Weixler B, Ramser M, Warschkow R, et al. The Value of Sentinel Lymph Node Mapping for the Staging of Node-Negative Colon Cancer: Propensity Score and Mediation Analyses. Annals of Surgery Open. 2021;2(3):e084. doi:10.1097/AS9.0000000000000084.
- Dias AR, Pereira MA, Mello ES, Cecconello I, Ribeiro-Jr U, Nahas SC. Carnoy’s solution increases lymph nodes count in colon cancer specimens when compared to formalin fixation: a randomized trial. Arq Bras Cir Dig. 2022;35:e1656. doi:10.1590/0102-672020210002e1656.
- Seymour MT, Morton D. International FOxTROT Trial Investigators. FOxTROT: an international randomised controlled trial in 1052 patients (pts) evaluating neoadjuvant chemotherapy (NAC) for colon cancer. J Clin Oncol. 2019;15(suppl):3504–3504.
- Karoui M, Rullier A, Piessen G, et al. Perioperative FOLFOX 4 Versus FOLFOX 4 Plus Cetuximab Versus Immediate Surgery for High-Risk Stage II and III Colon Cancers: A Phase II Multicenter Randomized Controlled Trial (PRODIGE 22). Ann Surg. 2020;271(4):637-645. doi:10.1097/SLA.0000000000003454.
- Chalabi M, Fanchi LF, Dijkstra KK, et al. Neoadjuvant immunotherapy leads to pathological responses in MMR-proficient and MMR-deficient early-stage colon cancers. Nat Med. 2020;26(4):566-576. doi:10.1038/s41591-020-0805-8.
- Matsumoto A, Shinohara H, Suzuki H. Laparoscopic and open surgery in patients with transverse colon cancer: short-term and oncological outcomes. BJS Open. 20216;5(5):zrab078. doi:10.1093/bjsopen/zrab078.
- Cuk P, Kjær MD, Mogensen CB, Nielsen MF, Pedersen AK, Ellebæk MB. Short-term outcomes in robot-assisted compared to laparoscopic colon cancer resections: a systematic review and meta-analysis. Surg Endosc. 2022;36(1):32-46. doi:10.1007/s00464-021-08782-7.
- Thong MSY, Jansen L, Chang-Claude J, Hoffmeister M, Brenner H, Arndt V. Association of laparoscopic colectomy versus open colectomy on the long-term health-related quality of life of colon cancer survivors [published correction appears in Surg Endosc. 2021 Aug;35(8):4900]. Surg Endosc. 2020;34(12):5593-5603. doi:10.1007/s00464-019-07360-2.
- Du Q, Yang Y, Zhang J, Liu X, Wang Y, Yang L. Laparoscopic versus open left hemicolectomy for left-sided colon cancer: protocol for a systematic review and meta-analysis. BMJ Open. 2022;12(6):e062216. doi: 10.1136/bmjopen-2022-062216.
- Yang SY, Kim MJ, Kye BH, et al. Prospective study of oncologic outcomes after laparoscopic modified complete mesocolic excision for non-metastatic right colon cancer (PIONEER study): study protocol of a multicentre single-arm trial. BMC Cancer. 2020;20(1):657. doi:10.1186/s12885-020-07151-2.
- Dohmoto M. New method: endoscopic implantation of rectal stent in palliative treatment of malignant stenosis. Endosc Dig. 1991;3:1507–1512
- Kye BH, Kim JH, Kim HJ, Lee YS, Lee IK, Kang WK, Cho HM, Ahn CH, Oh ST. The optimal time interval between the placement of self-expandable metallic stent and elective surgery in patients with obstructive colon cancer. Sci Rep. 2020;10(1):9502. doi:10.1038/s41598-020-66508-6.
- Kim HJ, Choi GS, Park JS, Park SY, Jun SH. Higher rate of perineural invasion in stent-laparoscopic approach in comparison to emergent open resection for obstructing left-sided colon cancer. Int J Colorectal Dis. 2013;28(3):407-414. doi:10.1007/s00384-012-1556-x.
- Han JG, Wang ZJ, Zeng WG, Wang YB, Wei GH, Zhai ZW, Zhao BC, Yi BQ. Efficacy and safety of self-expanding metallic stent placement followed by neoadjuvant chemotherapy and scheduled surgery for treatment of obstructing left-sided colonic cancer. BMC Cancer. 2020;20(1):57. doi:10.1186/s12885-020-6560-x.
- Dillon J, Mills AN, Pawloski KR, Scribetta N, Greenstein A. Arterial-colonic fistula secondary to colonic stent erosion into the left external iliac artery. J Surg Case Rep. 2023;2023(1):rjac615. doi:10.1093/jscr/rjac615.
- Li W, Jin X, Liang G. The efficacy of endoscopic stenting combined with laparoscopy in the treatment of left colon cancer with obstruction. J Cancer Res Ther. 2019;15(2):375-379. doi:10.4103/jcrt. JCRT_111_18.
- Pattarajierapan S, Manomayangoon C, Tipsuwannakul P, Khomvilai S. Comparison of colonic stenting and stoma creation as palliative treatment for incurable malignant colonic obstruction. JGH Open. 2022;6(9):630-636. doi:10.1002/jgh3.12800.
- Mesri M, Hitchman L, Yiaesemidou M, Quyn A, Jayne D, Chetter I. Protocol: The role of defunctioning stoma prior to neoadjuvant therapy for locally advanced colonic and rectal cancer - A systematic review. PLoS One. 2022;17(9):e0275025. doi:10.1371/journal.pone.0275025.
- Kuwai T, Tamaru Y, Kusunoki R, et al. Long-term outcomes of standardized colonic stenting using WallFlex as a bridge to surgery: Multicenter prospective cohort study. Dig Endosc. 2022;34(4):840-849. doi:10.1111/den.14137.
- Cirocchi R, Arezzo A, Sapienza P, et al. Current Status of the Self-Expandable Metal Stent as a Bridge to Surgery Versus Emergency Surgery in Colorectal Cancer: Results from an Updated Systematic Review and Meta-Analysis of the Literature. Medicina (Kaunas). 2021;57(3):268. doi:10.3390/medicina57030268.
- Huiskens J, Bolhuis K, Engelbrecht MR, De Jong KP, Kazemier G, Liem MS, Verhoef C, de Wilt JH, Punt CJ, van Gulik TM; Dutch Colorectal Cancer Group. Outcomes of Resectability Assessment of the Dutch Colorectal Cancer Group Liver Metastases Expert Panel. J Am Coll Surg. 2019 Dec;229(6):523-532.e2. doi: 10.1016/j.jamcollsurg.2019.08.1445. Epub 2019 Sep 11. PMID: 31520695.
- Hellingman T, Galjart B, Henneman JJ, et al. Limited Effect of Perioperative Systemic Therapy in Patients Selected for Repeat Local Treatment of Recurrent Colorectal Cancer Liver Metastases. Annals of Surgery Open. 2022;3(2):pe164. doi:10.1097/AS9.0000000000000164
- Nierop PM, Höppener DJ, Buisman FE, et al. Preoperative systemic chemotherapy alters the histopathological growth patterns of colorectal liver metastases. J Pathol Clin Res. 2022;8(1):48-64. doi: 10.1002/cjp2.235.
- Sommariva A, Tonello M, Coccolini F, et al. Colorectal Cancer with Peritoneal Metastases: The Impact of the Results of PROPHYLOCHIP, COLOPEC, and PRODIGE 7 Trials on Peritoneal Disease Management. Cancers (Basel). 2022;15(1):165. doi:10.3390/cancers15010165.
- Pereira F, Serrano A, Manzanedo I, et al. GECOP-MMC: phase IV randomized clinical trial to evaluate the efficacy of hyperthermic intraperitoneal chemotherapy (HIPEC) with mytomicin-C after complete surgical cytoreduction in patients with colon cancer peritoneal metastases. BMC Cancer. 2022;22(1):536. doi:10.1186/s12885-022-09572-7.
- Hübner M, Somashekhar SP, Teixeira Farinha H, et al. Treatment Response After Pressurized Intraperitoneal Aerosol Chemotherapy (PIPAC) for Peritoneal Metastases of Colorectal Origin. Annals of Surgery Open. 2022;3(4):e203. doi:10.1097/AS9.0000000000000203.
- Lotfollahzadeh S, Recio-Boiles A, Cagir B. Colon Cancer. In: StatPearls. Treasure Island (FL): StatPearls Publishing; December 3, 2022.
- Reali C, Bocca G, Lindsey I, Jones O, Cunningham C, Guy R, George B, Boyce S. Influence of incorrect staging of colorectal carcinoma on oncological outcome: are we playing safely? Updates Surg. 2022;74(2):591-597. doi:10.1007/s13304-021-01095-3.
- Wetterholm E, Rosén R, Rahman M, Rönnow CF. CT is unreliable in locoregional staging of early colon cancer: A nationwide registry-based study. Scand J Surg. 2023;112(1):33-40. doi:10.1177/14574969221132648.
- Gustafsson UO, Scott MJ, Hubner M, et al. Guidelines for Perioperative Care in Elective Colorectal Surgery: Enhanced Recovery After Surgery (ERAS®) Society Recommendations: 2018. World J Surg. 2019;43(3):659-695. doi:10.1007/s00268-018-4844-y.
- Matsuda T, Yamashita K, Hasegawa H, Oshikiri T, Hosono M, Higashino N, Yamamoto M, Matsuda Y, Kanaji S, Nakamura T, Suzuki S, Sumi Y, Kakeji Y. Recent updates in the surgical treatment of colorectal cancer. Ann Gastroenterol Surg. 2018;2(2):129-136. doi:10.1002/ags3.12061.
- Pisano M, Zorcolo L, Merli C, et al. 2017 WSES guidelines on colon and rectal cancer emergencies: obstruction and perforation. World J Emerg Surg. 2018;13:36. doi:10.1186/s13017-018-0192-3.