This article presents the direct esthetic restorations characteristics using adhesive materials in the posterior area. The adhesive materials, the different types of modified cavities, the special aspects of their outline, walls, internal angles and external edges are presented, so that they benefit from the corresponding properties of the used materials. Aspects of the adhesive work technique, such as dam isolation or the use of modern coronal conformation systems, are also discussed.
Restaurările estetice adezive directe în zona laterală
Direct posterior esthetic adhesive odontal restorations
First published: 20 februarie 2024
Editorial Group: MEDICHUB MEDIA
DOI: 10.26416/ORL.62.1.2024.9218
Abstract
Rezumat
Acest articol prezintă caracteristicile restaurărilor estetice realizate cu materiale aderente la nivelul dinţilor laterali. Sunt prezentate materialele adezive, diferitele tipuri de cavităţi modificate, aspectele speciale ale conturului, pereţilor, unghiurilor interne şi marginilor exterioare ale acestora, astfel încât să beneficiem de proprietăţile corespunzătoare ale materialelor utilizate. De asemenea, sunt discutate aspecte ale tehnicii de lucru adezive, cum ar fi izolarea cu digă sau utilizarea unor sisteme moderne de conformare coronară.
Introduction
With the passage of years and the massive advancement of techniques and materials in dentistry, both doctors and patients have a choice between a multitude of materials that are used to restore a tooth affected by dental caries, to restore a tooth that has suffered a trauma, or to treat different types of noncarious loss of dental hard substance. All modern materials have in common the ability to bond to tooth structure.
Nowadays, adhesive materials are used, which present both retention through chemical mechanisms, such as glass ionomer cements, as well as the best known, the materials of choice in modern dentistry, the resin based materials, which use adhesive systems(1). Composite resin is a material consisting of two main components:
-
the organic component is a matrix represented by acrylic compounds;
-
the inorganic component (filler), consisting of a mixture of powders with a content similar to that of glass – different oxides (silicon, aluminum, quartz etc.).
Also, it contains coupling agent (silane), initiator system, stabilizers, and pigments.
When the process of composite setting reaction (poymerization reaction) takes place, the obtained material has properties similar to those of dental tissues, regarding hardness, elasticity, resistance, chemical and thermal isolation of the pulp and color and translucency. Due to the presence of the organic phase, resin composites bond mechanical (penetration of resin and formation of resin tags), chemically through adsorption to the organic and inorganic components of enamel and dentin, diffusion (precipitation of substances on the tooth surfaces to which resin monomers can bond), but this is only possible using an adhesive system(2).
The components of an adhesive system are:
-
the phosphoric acid – for demineralization of hard dental tissues and for creating microretentions in organic matrix of enamel or dentine;
-
the primer – with the role of hydrating the organic matrix, restoring the three-dimensional architecture of the dentine collagen network;
-
bonding – penetrating among the previously created microretentions, forming chemical bonds in both directions, with the dental tissue and with the composite resin.
In the category of currently adhesive materials, there are also hybrids between these two large classes, namely compomers, glass ionomer cements modified with the addition of resins, and giomers, in order to improve their mechanical or chemical properties and adhesion(3).
Direct esthetic adhesive restorations in posterior area
We can say that the use of adhesive materials in the case of direct restoration techniques has as its first advantage the physiognomic aspect, due to the esthetic improvement obtained compared to conventional restorations with amalgam(4).
However, the main change that modern adhesive materials have brought to the treatment principles of operative dentistry, both in the anterior and posterior areas, is the modified design of the cavities. The specificity of adhesive dentistry is minimal intervention, respectively minimally invasive cavities(5). Thus, the dental sacrifice is reduced, it is not necessary to prepare a retentive cavity as in the case of dental amalgam, the simple removal of the affected enamel and necrotic dentin being sufficient. It is obvious that the other classic Black’s treatment principles should not be excluded, namely preventive extension or resistance, but the approach is different compared to conventional restorations. Practically, in dentistry, the “extension for prevention” paradigm has changed after dental adhesion invention in “prevention of extension”(6).
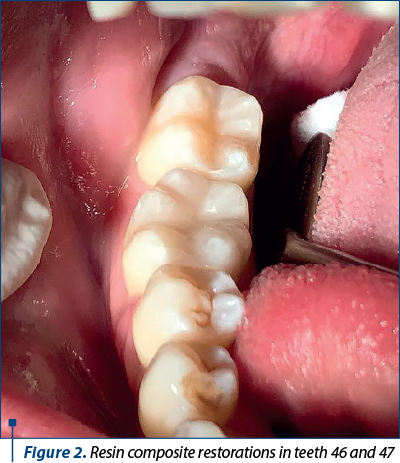
The configuration of the cavities in the lateral areas for adhesive materials presents common characteristics with those of classic cavities in terms of the complete excision of the tissues affected by the dental caries, but the shape and outline of the cavities are modified in a minimally invasive way(7).
The class I cavity will have a contour resulting from the excision of the necrotic and affected enamel. The vestibular and oral lateral walls will be convergent towards the occlusal, and the mesial and distal ones will be slightly convergent or parallel towards the occlusal. The cavity can have reduced sagittal or transverse dimensions of 1-1.5 mm, with a depth of at least 1.5-2 mm. The internal dentine angles are rounded, and the cavo-surface angles are 90 degrees or obtuse to avoid stress concentration and the initiation of cracks. Even though modern dentistry is minimally invasive, conservative with respect to the dental tissues, in the clinical situation where there are demineralized areas in relation to the carious lesion, they are included in the outline of the created cavity, following the principle of preventive extension. The patient’s cario-susceptibility must always be taken into account, guiding us towards a stricter approach regarding this rule, without admitting concessions.
In the situation when, following the cavity preparation, its walls are undermined, the dentist must evaluate the risk of their fracturing and, depending on the clinical situation, adopt one of the following options: lining with glass ionomer cement type material (“sandwich” technique – the most used current direct restoration technique), or sometimes it may be necessary to reduce their height to the area that ensures sufficient mechanical resistance. Regardless of the chosen therapeutic approach, knowledge and use of composite layering techniques, so as to reduce its shrinkage, are mandatory.
The layering application also reduces the tension that occurs at the restorative material-dental structure interface. The result of polymerization contraction in composite resins is the damage to the adhesive interface and the consequent appearance of marginal nano, micro and macro infiltration areas(8). To the same extent, however, the tensions inside the composite resin are exerted on the walls of the cavity. When these are thin, cusp flexure appears, which is a linear movement of the cusps tips due to the polymerization shrinkage stress. Enamel microcracks may appear especially at the cervical level, as a result leading to subsequent coronary fracture. The phenomenon of cuspal deflection is especially accentuated and frequently encountered in upper premolars, when they present voluminous restorations. Their coronal morphology, which presents accentuated cusps and a deep intercuspid groove, predisposes to cusp flexure(9).
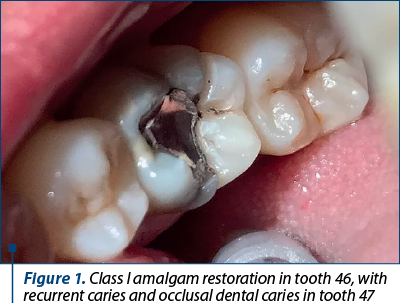
The recurrent caries associated with an existing restoration, especially when is a nonadhesive one, like amalgam, usually bring the challenge of a primary important loss of hard dental substance, which produces stress in the tooth structure, given that the cavity was prepared, according to Black, with great sacrifice of hard tissues. Added to this is the loss of substance through marginal secondary caries or residual caries, frequently resulting in cavities with strongly weakened walls. In direct adhesive restorations, however, they are preserved and can be successfully rebuilt.
Regarding the class II modified cavities for adhesive restorations, they will be prepared as conservatively as possible, respecting the above discussed principles, without including the centric stops in the cavity contour.
The interdental surfaces represent retentive areas for the bacterial microfilm, difficult to be cleaned, with increased chances of consecutive dental caries appearance. Thus, in order to minimize the patient’s discomfort during the treatment, increase the lifespan of the restoration and at the same time to facilitate the clinician’s effort, the restoration techniques have been perfected, being now available new minimally invasive preparation methods associated with adhesive materials(10). If the dental caries is shallow and located on the proximal surface, and the marginal ridge is intact, the cavity can have one of the following forms:
-
The “modified box” type proximal cavity is indicated in the case of a direct access to the affected proximal face or when the lesion can be instrumented through a face-to-face preparation of adjacent tooth, and its restoration can be performed both with glass ionomer cement, as well as with resin composite.
-
The “tunnel” type cavity, specific to superficial proximal dental caries situated below the contact point, requires an approach from the occlusal side, keeping a distance of 2 mm from the marginal ridge, which must be preserved. A gradual widening of the cavity is carried out to allow the complete removal of the affected tissues, protecting the adjacent tooth with a metal matrix placed interdentally.
-
The “horizontal slot” cavity, where access is facial and oral, is located below the contact point and is indicated in the case of incipient dental caries.
The well-known vertical “slot” type cavity, in which access is achieved through the marginal ridge, is indicated in situations where the dental caries is superficial or of medium depth, and is near the marginal ridge. This type of approach is currently the most frequently used in composite restorations for proximal lesions in the posterior area. Compared to conventional restorations, horizontal retention cavity is no longer indicated, although this is sometimes necessary in special situations, such as deep proximal dental caries, or when the patient presents parafunctions with important occlusal forces which led to the previous loss of the adhesive restoration (bruxism), in patients with high cario-susceptibility, or when there is simultaneous occlusal and proximal carious hard dental structure loss.
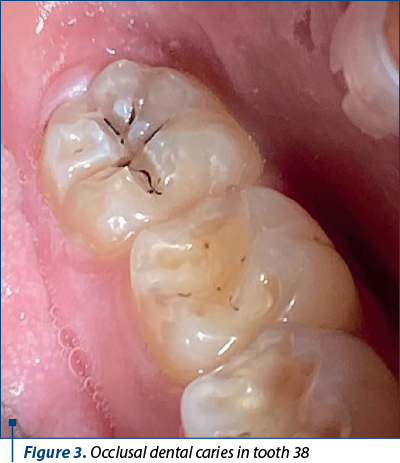
As a conclusion, the aspects related to the preventive extension rule for proximal cavities that will be adhesive restored are limited to the complete removal of demineralized enamel along the contour of the cavity, even though it is in the area of contact with the adjacent tooth, and the challenges related to the resistance of the walls are similar with those from class I (with deficient strategic dental substance, respectively absent marginal ridges in this situation).
The adhesive cervical restorations in the posterior area present the same outline dictated by the expansion of the caries process, with rounded internal and external angles and bevels in the areas where this is possible and necessary(11).
Another particular aspect of the adhesive esthetic restorations is the need to use for moisture control the isolation dam system, so that the specific properties of used materials can be obtained, and the process of dentin hybridization can take place in optimal conditions. In this way, the marginal sealing, which is the key point in the longevity of an adhesive restoration, is correctly obtained. The use of the modern isolation method, in addition to optimizing the properties of restorative materials, presents other advantages, among which we list: protecting the patient’s soft tissues from contact with different substances, whether they are represented by irrigation liquids or dental materials; prevention of inhalation or accidental aspiration by the patient of small instruments or various substances. Also, the isolation of the operating field from saliva, during the therapeutic procedures, ensures increased visibility, so we have efficiency and accuracy in complying with the treatment protocol. That is why, even though the dentist often applies the dam system before initiating the cavity preparation stage only in the case of profound dental caries with high risk of accidental opening of pulp chamber, it is more cautious and desirable that the dam be applied from the beginning in all clinical situations where adhesive restoration is necessary(12).
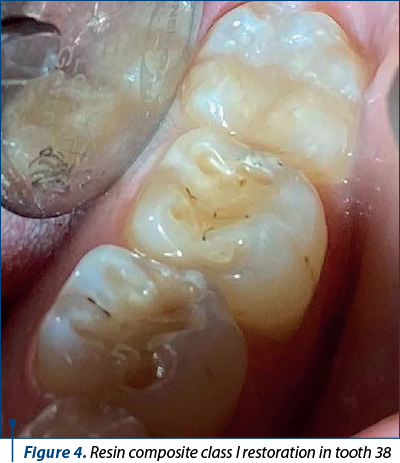
Direct proximal restorations in the posterior area always raise problems related to the correct restoration of the contact point. Classically, the matrices used were of the Ivory (sectional) and Toffelmyre (circular) types, and they allow a correct restoration(13). With the intensive development of dentistry, countless matrix systems have been developed, and they allow to obtain an adequate marginal seal, a correct proximal contour and contact point. The use of modern Palodent (Dentsply Sirona), Palodent Plus (Dentsply Sirona), Supermat Matrix (Kerr), Garrison, Unimatrix (TDV Deantal), and many other available systems, along with flowable, condensable and bulk composites, offer the possibilities for an accurate proximal esthetic restoration(14).
Conclusions
Modern esthetic adhesive materials allow minimally invasive direct restoration of dental caries, but knowledge and rigorous application of the specific treatment protocol are mandatory. The first condition that must be respected in order to ensure the longevity of the adhesive restoration is to prepare a modified cavity, with special characteristics of the outline, walls, internal angles and external edges, so that it benefits from the appropriate properties of the materials used. This is associated with the particularities of therapeutic maneuvers for adhesive techniques: isolation with a dam or the use of modern systems for coronal conformation. In this way, high-quality esthetic adhesive conservative restorations can be achieved.
Acknowledgements. For this article, all the authors have equal contributions.
Corresponding author:
Irina-MariaGheorghiu
E-mail: igheorghiu@hotmail.com
Conflict of interest: none declared.
Financial support: none declared.
This work is permanently accessible online free of charge and published under the CC-BY licence.

Bibliografie
- Perdigão J, Araujo E, Ramos RQ, Gomes G, Pizzolotto L. Adhesive dentistry: Current concepts and clinical considerations. J Esthet Restor Dent. 2021;33(1):51-68.
- Dressano D, Salvador MV, Oliveira MT, Marchi GM, Fronza BM, Hadis M, Palin WM, Lima AF. Chemistry of novel and contemporary resin-based dental adhesives.
- J Mech Behav Biomed Mater. 2020 Oct;110:103875.
- Zhou W, Liu S, Zhou X, Hannig M, Rupf S, Feng J, Peng X, Cheng L. Modifying Adhesive Materials to Improve the Longevity of Resinous Restorations. Int J Mol Sci. 2019;20(3):723.
- Mackenzie L, Shortall A, Burke T, Parmar D. Posterior composites: An update. Dental Update. 2019;46(4):323-343.
- Thalacker C. Dental adhesion with resin composites: a review and clinical tips for best practice. Br Dent J. 2022;232(9):615-619.
- Larson TD. Extension for prevention: margin placement. Northwest Dent. 2021;91(2):12-16, 17, 19.
- Burke T. Enhancing adhesive restoration effectiveness. Dental Update. 2020;47(7):545-547.
- Hervas-García A, Martínez-Lozano MA, Cabanes-Vila J, Barjau-Escribano A, Fos-Galve P. Composite resins. A review of the materials and clinical indications. Med Oral Patol Oral Cir Buc. 2006;11:E215-20.
- Gheorghiu IM, Scărlătescu S, Perlea P, Temelcea A. Specific aspects of the dental restorative treatments in premolars. Romanian Journal of Stomatology. 2017;63(2):88-93.
- Frencken JE. Minimal intervention dentistry for managing dental caries – a review. Int Dent J. 2012;62(5):223–243.
- Lührs AK, Jacker-Guhr S, Günay H, Herrmann P. Composite restorations placed in non-carious cervical lesions – Which cavity preparation is clinically reliable? Clin Exp Dent Res. 2020;6(5):558-567.
- Mohan MC, Geetha P, Soman D, et al. The Effect of Salivary Contamination on the Shear Bond Strength of Seventh- and Eighth-generation Adhesive Systems. Int J Clin Pediatr Dent. 2023;16(S-1):S63-S66.
- Cohen R, Razzano M. Successful Proximal Management of the Minimal Class 2 Direct Composite Restoration. Inside Dentistry. 2009 Feb;5(Issue 2).
- Gheorghiu IM, Mitran L, Mitran M, Scărlătescu S, Iliescu AA, Perlea P, Nistor OA. Special aspects of direct restoration in posterior teeth. ORL.ro. 2023;60(3):48-51.